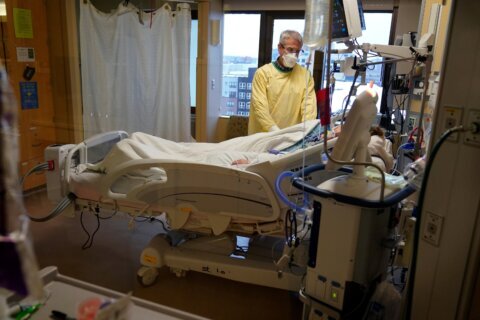
Recovery from COVID-19 can continue for many weeks or even months after the infection passes. Whether you’re obviously deconditioned after a lengthy hospitalization or coping with more subtle effects of a seemingly ‘mild’ case, it can be challenging.
Restoring muscle mass and strength, physical endurance, breathing capacity, mental clarity emotional well-being and daily energy levels are important for former hospital patients and COVID long-haulers alike. Below, experts weigh in on what COVID-19 recovery involves.
Comprehensive Recovery Plan
Individual recovery needs vary depending on the patient and their COVID-19 course. Major health areas that are frequently affected and must be addressed include:
— Strength and mobility. Hospitalization and virus infection itself can erode muscle strength and mass. Immobility from bedrest in the hospital or at home can be gradually reversed.
— Endurance. Fatigue is a huge problem with long COVID, requiring careful activity pacing.
— Breathing. Lung effects from COVID pneumonia may persist. Medical treatments plus physical therapy can improve breathing.
— Functional fitness. When activities of daily life like lifting household objects are no longer performed with ease, function can be restored.
— Mental clarity/emotional equilibrium. So-called brain fog makes it hard to work or concentrate, and the effect is real, not imaginary. Going through a serious illness, prolonged hospitalization and persistent health problems is upsetting. Support from therapy helps.
— General health. The pandemic too often overshadowed concerns such as cancer care, dental checkups or routine screenings, but overall health issues also require attention.
[See: Mind-Blowing Benefits of Exercise.]
Strength and Mobility
When the muscular-skeletal system takes a hit from COVID-19, it reverberates throughout the body. “Muscle plays a critical role,” says Suzette Pereira, a muscle health researcher with Abbott, a global health care company. “It accounts for roughly 40% of our body weight and is a metabolic organ that works other organs and tissues in the body. It provides nutrients to critical organs during times of illness, and losing too much can put your health at risk.”
Unfortunately, without intentional focus on muscle health, muscle strength and function can drastically deteriorate in COVID-19 patients. “It’s a Catch-22,” says Brianne Mooney, a physical therapist at the Hospital for Special Surgery in New York City. She explains that lack of movement significantly exacerbates muscle loss, while movement can feel impossible with the energy-draining disease. To make matters worse, muscle atrophy increases fatigue, making movement even less likely.
Patients can lose up to 30% of muscle mass in the first 10 days of intensive care unit admission, research shows. Patients hospitalized due to COVID-19 are usually in the hospital for at least two weeks, while those who go into the ICU spend about a month and a half there, says Dr. Sol M. Abreu-Sosa, a physical medicine and rehabilitation specialist who works with COVID-19 patients at Rush University Medical Center in Chicago.
[Read: Telemedicine Explodes to the Forefront Amid COVID-19.]
Maintaining Muscle Strength
Even in the best of conditions, for those experiencing strong COVID-19 symptoms, it’s likely that some muscle loss will occur. However, patients can greatly influence the degree of muscle loss and, in mild cases, may be able to maintain muscle health, says Mooney, a member of the team that created the Hospital for Special Surgery’s COVID-19 nutritional and physical rehabilitation guidelines.
These strategies can help protect muscle, strength and overall health during recovery:
— Move as you’re able.
— Add resistance.
— Prioritize nutrition.
Move as you’re able
“The sooner you move, the better,” Abreu-Sosa says, explaining that, in the hospital, the COVID-19 patients she works with have three hours of physical therapy five days per week. “Here in the hospital, we are starting exercise even on the day of admission if vitals are stable. Even in patients who are intubated, we work on passive raise of motion, raising their arms and legs and positioning muscles.”
Once home, Mooney recommends people get up and move every 45 minutes or so. Walking, performing acts of daily living like bathing and dressing as well as structured exercises such as cycling and squats are beneficial.
“Any physical activity should be based on symptoms and current levels of function,” she says, explaining that the goal is to engage the muscles of the body without exacerbating any symptoms. Fatigue, shortness of breath and dizziness are all cause to stop exercise.
Add resistance
When integrating movement into your recovery routine, prioritize resistance-based exercises that challenge your body’s largest muscle groups, Mooney recommends. She says that completing three 15-minute workouts per week is a great starting point, and patients can increase frequency and duration as recovery progresses.
Take special care to focus on the hips and thighs as well as back and shoulders, as these muscle groups tend to lose the most strength in COVID-19 patients and have wide-reaching effects on the ability to stand, walk and perform everyday tasks, Abreu-Sosa says.
To strengthen the lower body, try exercises such as squats, glute bridges and side steps. For the upper body, incorporate row and shoulder-press variations. Your body weight, light dumbbells and resistance bands all make great at-home resistance gear, Mooney says.
Prioritize nutrition
“Protein is needed to build, repair and maintain muscle, but also to support the production of antibodies and immune system cells,” Pereira says. Unfortunately, protein intake is often lower than it should be in COVID-19 patients. “Aim for 25 to 30 grams of protein at every meal if possible, by eating meats, eggs and beans or using an oral nutrition supplement,” she recommends.
Vitamin A, C, D and E and zinc are critical to immune function, but they also play a role in both muscle health and energy, Pereira says. She recommends incorporating milk, fatty fish, fruits and veggies and other plants like nuts, seeds and beans into your recovery diet. If you have trouble cooking for yourself at home, consider trying out healthy meal-delivery services to help you get a wide range of nutrients.
[READ: COVID-19 and Hearing Loss.]
Endurance
Pushing through fatigue and weakness can be counterproductive when you have long COVID. Respecting post-COVID fatigue is part of the path to recovery.
Excessive Fatigue
Fatigue is among the top symptoms that brings patients seeking physical therapy to the Johns Hopkins Post-Acute COVID-19 Team, says Jennifer Zanni, a cardiovascular and pulmonary clinical specialist at Johns Hopkins Rehabilitation at Timonium, in Maryland. “It’s not the type of fatigue necessarily that you’d see with someone who’s just become deconditioned or who has lost all this muscle strength,” she says. “It’s just symptoms that limit their ability to do their normal daily activities — their school or work activities.”
Pacing Yourself
A little too much activity can bring on disproportionate tiredness for people with post-COVID malaise. “Our treatment has to be very individualized to the patient, for example, if a patient presents and has what we term ‘post-exertional malaise,'” Zanni says. That, she explains, is when someone does a physical activity like exercise or even just a mental task like reading or being on a computer, and it causes fatigue or other symptoms to become much worse in the next 24 or 48 hours.
“If a patient has those types of symptoms, we have to be very careful about how we prescribe exercise, because you can actually make someone worse,” Zanni says. “So we may just be working on pacing and making sure they get through daily activities, like breaking things up into smaller tasks.”
What felt like a short, easy jaunt before COVID-19 can become a major stressor, patients may say. “It could be something small, like they walked a mile and can’t get out of bed for the next two days — so, way out of proportion to the activity,” Zanni says. “But it’s just like their available energy is very limited and if they exceed that it takes a long time to recover.”
Just as you do with money, spend your valuable energy wisely. By learning to pace yourself, you may prevent utter exhaustion from setting in.
Breathing
Respiratory complications like pneumonia can have long-term breathing effects. In addition, Abreu-Sosa notes that in the treatment of COVID-19, doctors sometimes use steroids with patients, as well as paralytic agents and nerve blocks in those requiring ventilators, all of which can speed muscle breakdown and weakness. In COVID-19 patients, this deterioration even includes the respiratory muscles that control inhalation and exhalation.
Breathing exercises are a standard part of recovery. A patient booklet created by Zanni and colleagues early in the pandemic outlines movement recovery phases. “Breathe deep” is the message in terms of breathing. Deep breathing restores lung function by using the diaphragm, the booklet notes, and encourages a restoration and relaxation mode in the nervous system.
— Beginning phase. Practice deep breathing on your back and on your stomach. Humming or singing incorporate deep breathing, as well.
— Building phase. While sitting and standing, consciously use deep breathing while placing your hands around the side of your stomach.
— Being phase. Deep breathe while standing and throughout all activities.
Aerobic training, such as sessions on a treadmill or exercise bike, is part of a comprehensive approach to building breathing capacity, overall fitness and endurance.
As the pandemic wore on, it became clear that persistent lung problems can complicate long-term recovery plans. “I do have some patients with ongoing lung problems, just because having COVID has caused some damage in their lungs,” Zanni says. “That can be very slow to resolve or in some cases permanent. Some patients need oxygen for a period of time. It just sort of depends how severe their illness was and how well they recovered.”
Rehab for a patient whose lungs are compromised takes a multidisciplinary approach. “We’re working with the physicians from a medical standpoint to optimize their lung functions,” Zanni says. For instance, she says, that could mean patients are using inhaler medication to allow them to exercise. “We also exercise in ways that they can tolerate. So if someone is having more shortness of breath, we may begin exercise more with interval training, meaning short periods of exercise with little rest breaks.”
Functional Fitness
Performing everyday tasks you used to take for granted, like walking downstairs or lifting household objects, is part of functional fitness. So is having the energy and ability to do your job.
For many employees, traditional expectations of working intently for hours on end are no longer realistic as they continue to recover from COVID-19.
After the initial bout with COVID-19, returning to work can be surprisingly difficult. “For a lot of people, work is challenging,” Zanni says. “Even sitting at a computer may not be physically taxing, but it can be cognitively taxing, which can (cause) just as much fatigue sometimes.”
Functional training allows people to return to meaningful activities in their lives, not just by building strength but also by using their bodies more efficiently. Learning proper movement patterns and strengthening key muscle groups can help restore balance and agility, coordination, posture and power to participate in family gatherings, outdoor activities like hiking or work routines such as sitting and working on a computer.
However, it may be impossible for some employees to resume normal work duties as usual. “Some people aren’t able to work at all because of their symptoms,” she says. “Some people are having to adjust their work schedules or work from home. Some people don’t have the ability to not work — they’re working but almost every day they’re going through their available energy, which is a tougher scenario.” That can be a challenge for many people who don’t have the luxury of not working or at least taking a break when they need one, she notes.
Some long-COVID care providers may help educate patients’ employers, for instance sending letters to inform them about long COVID, so they can better understand potential health effects and be more accommodating when needed.
Mental/Emotional Equilibrium
A well-rounded team of health care providers will ensure that your recovery plan is individualized, comprehensive and holistic, incorporating physical and mental health. As part of that, Zanni notes that many patients who are seen at the Hopkins PACT clinic receive screening for psychological and cognitive issues.
In a rehab bonus, patients have the opportunity to realize they’re not alone. Otherwise, it can be discouraging when employers, friends or even family members question whether you’re really still weak, tired or mentally or emotionally struggling when you know that’s truly the case. Part of long COVID rehab is receiving support and belief.
“A lot of my patients would say just having someone validate what they’re experiencing is probably a big thing,” Zanni says. “Because a lot of symptoms are what people are telling you and not what a lab test is showing.”
Zanni and colleagues see patients both as outpatients at the clinic or through telehealth, which can make access easier. Increasingly, medical centers are offering post-COVID programs for those with lingering issues. Your primary care provider may be able to recommend a program in your area, or you can check with local medical centers.
General Health
It’s important to keep in mind that a new health problem or symptom may be caused by something other than COVID-19. Multidisciplinary communication is crucial when patients are evaluated for long-COVID rehab, Zanni says.
With physical or cognitive changes, functional issues or symptoms of fatigue, clinicians must rule out non-COVID possibilities. As always, cardiac, endocrine, oncology or other pulmonary conditions can cause a multitude of overlapping symptoms. All this speaks to having good access to medical care, Zanni says, and the need for a thorough evaluation rather than just saying: This is all long COVID.
More from U.S. News
What Weakens the Immune System?
10 Healthy Drinks Rich in Electrolytes
9 Exercises Men Should Do Every Day
How to Regain Strength After COVID-19 originally appeared on usnews.com
Update 04/29/22: This story was previously published at an earlier date and has been updated with new information.