


WASHINGTON — Every year in the U.S., 20,000 people need a stem-cell transplant to help them beat cancer. With only a one-in-four chance of finding a match among relatives, these patients are generally left to count on strangers.
In December, I became one of those strangers.
The journey began earlier this decade, when I did a random swab for stem-cell donations at a Baltimore Jewish community center.
One day seven years later, my phone was full of text messages and voice mails. They were from Gift of Life, a national bone marrow registry. Apparently, I was a match for a 52-year-old man with cancer. Would I be interested in donating stem cells?
There was no way I could say no. My husband is a pediatric oncologist. I knew some of his young patients were “saved” by such a procedure. (It’s called a peripheral stem cell transplant: My stem cells would be extracted, then would go into the recipient’s blood and eventually make their way into his bone marrow.)
I was excited to help but nervous. The last two times I tried to give blood I nearly passed out. I wasn’t overly confident this would go any better.
Following a full physical and multiple blood tests, doctors at Georgetown University Medical Center confirmed I was in excellent health, and a December date was set for the collection of my stem cells.
The preparation
The actual process began five days before the donation. A nurse arranged by Gift of Life arrived at my home to take my blood pressure, administer injections, and make sure I felt fine afterwards.
It was explained to me that the drug Neupogen would stimulate the growth of more stem cells in my body and push stem cells out of my marrow and into my blood stream, where they would be collected.
The collection would take place right after my fifth and final injection — the day of the procedure.
I had been warned that some donors feel sick from the medication, especially when it’s close to the date of collection. That’s what happened to me. My husband, Dr. Jason Fixler, calmed my nerves, reassuring me the chest pains and flu-like symptoms were normal.
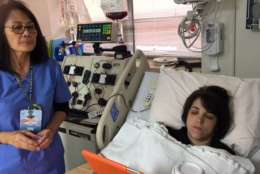
And then the big day arrived: Dec. 20. I checked into MedStar Georgetown University Hospital, where the Gift of Life’s Lindsay Katz was waiting for me with a large orange blanket and socks.
Gift of Life, she said, wants donors to feel welcome and comfortable. The registry was founded by Jay Feinberg, a man whose life was saved by a transplant. “Because of that, he likes to make sure all of our donors feel appreciated and are taken care of,” Katz said.
After a final shot of Neupogen — and a couple painful needle sticks for an IV — I was ready to go.
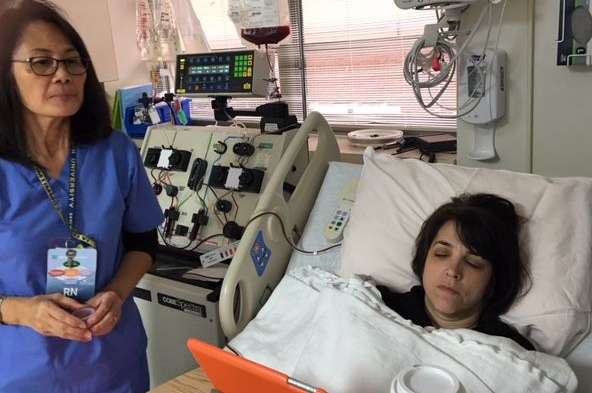
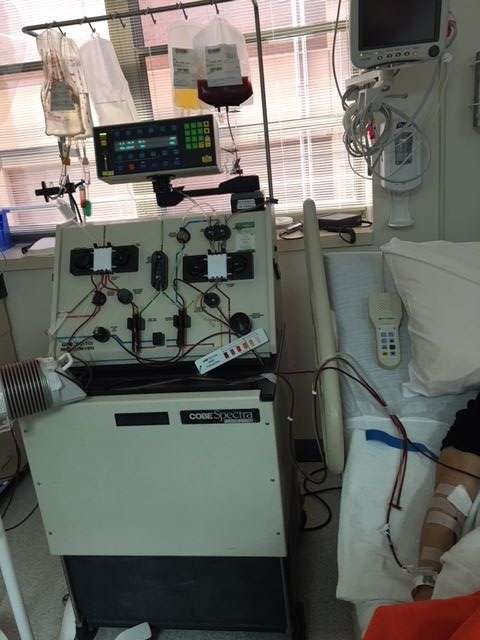
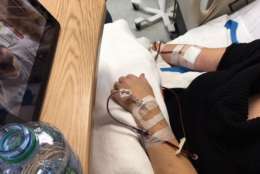
After I got comfortable, nurse Marjorie Cruz hooked me up to an Apheresis machine, which would separate the stem cells from my blood.
I would have to be immobile for the next six hours. (That included no bathroom trips.) Fortunately, I had an iPad, my husband and some good-natured nurses with me to pass the time.
“When you are on the machine, we use blood thinner,” the nurse explained. “What happens to you then is when you are getting this, it lowers your calcium level, so some people will have tingling around the lips, nose or fingertips. Some donors will also get a vibration feeling.”
I did feel strong vibrations in my legs, but only minor discomfort.
Dr. Corina Gonzales, director of the bone marrow and collection program at MedStar, oversaw the collection. It can be hard to find a match, she said: If someone has a sibling, there’s a 25 percent chance that that sibling is a match.
Not everyone has a sibling, however, “so we resort to people that are unrelated to the donor pool to find a match,” Gonzales said.
A stranger’s last chance
My husband had warned me I might be this patient’s last chance.
“Typically a good transplant patient is a male or a female patient that’s never had kids, and was young [i.e., under 40], and that wasn’t you,” he said. “So obviously, you were one of the last choices he had.”
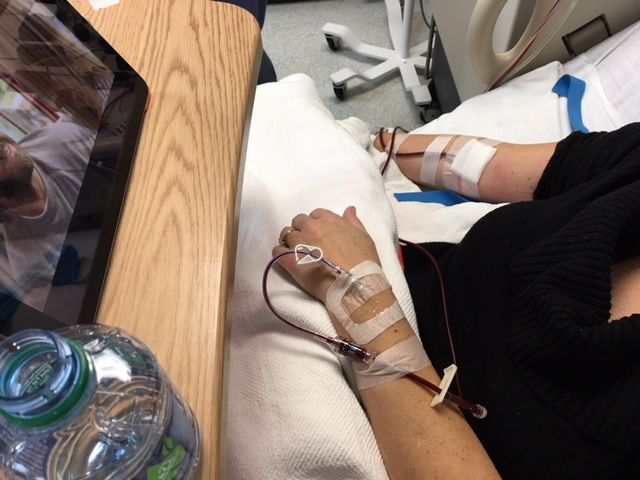
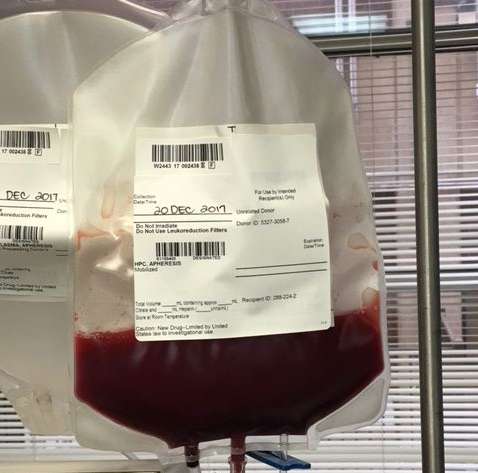
For six hours, I lay on a hospital bed while a machine beeped and slowly pulled out blood, removed the stem cells out of that blood, then returned the blood to me through the other arm. Eventually, the small pouch hanging near my bed was filled with my stem cells.
As I was unhooked, a courier arrived to whisk away my stem cells. I was told the patient would get the transplant the very next day. I’ll find out about the patient’s condition in a couple of months. (I still don’t know who he is, or even where he lives.) If he does well, Gift of Life will facilitate a meeting in about a year if he is interested.
Heading home on the train after the procedure, I felt grateful to have survived, hopeful that I helped someone, and happy to set a good example for my two children.
When people ask me about it, I tell them if I can do it, so can they. Throughout the procedure, I kept in mind Lindsay Katz’s words about the procedure’s lifesaving potential: “They are really saving peoples’ lives,” she said. “It’s not just saying your money will go somewhere and help someone. This is physically saving someone’s life, rebooting their immune system — the gift of life.”
Interested in giving a “gift of life”? Visit the registry’s website to find out where you can get swabbed to get onto an international database.