WASHINGTON — The doctor still remembers the visit well. The family walks into his office, young pitcher in tow, asking to get Tommy John surgery for his elbow, because they heard it will make it stronger. When did the elbow start hurting, the doctor asks. The elbow doesn’t hurt, they say. The elbow’s not injured.
The doctor tells the family they have 10 minutes to vacate the office before he calls Child Protective Services.
The doctor is Wiemi Douoguih, the team doctor for the Washington Nationals up through the 2015 season, now the medical director of MedStar Sports Medicine for the Washington region who serves as the medical director for both the Washington Wizards and Washington Capitals. He’s performed Tommy John surgery roughly 200 times, but sees the misconceptions about the surgery all the time.
So does another doctor, one with a familiar name.
“I don’t think there’s much respect for the surgery anymore,” Dr. Tommy John — son of the big leaguer after whom the surgery was named, who runs a performance and healing center in San Diego — told WTOP. “Nobody has any clue. Nobody has any idea.”
Douoguih and John are on the front lines of a national injury crisis. While 25 percent of active big leaguers have had the surgery, the number of young athletes 15 to 19 years old receiving the surgery has skyrocketed from 31 percent of all procedures in 2010 to 57 percent in 2016, with no signs of abating.
Perhaps it’s a nomenclature problem. The term “Tommy John” is tossed around so casually in the baseball world these days without even the word “surgery” attached to it. But that’s what it is, a surgery — and a major reconstructive one at that. Only about 80 percent of recipients return to play at their previous level, and even that number can be deceptive, as it only accounts for someone who comes back to throw a single pitch at their former level.
Might John himself have set an unrealistic expectation with his incredible recovery? He made it back in one year and one day, setting the bar for recovery at 12 months. But that has proved to be more like the optimum recovery time than the norm. Both Dr. John and Dr. Douoguih suggest a time window of 12 to 18 months is more appropriate.
“Whether they take 12 or 18 months doesn’t necessarily reflect how they’re going to do long-term,” said Douoguih. “The key is, you just don’t want to push them through pain that may be injuring the ligament in a way that’s irreversible.”
“Just because Tommy John came back in 12 months and one day, does not mean that everyone who has it should be in the 12-month range,” said John. “That’s the hard part of medicine, is that we confine everything to protocols and guidelines and milestones.”
***

You can’t talk about Tommy John surgery in Washington and not talk about Stephen Strasburg. The fallout and handling of his post-surgery career has been the most exhaustive sports topic in this city this decade, especially as more and more pitchers face the same recovery challenges, with mixed results.
The 200-inning starter is something of a rarity these days. The number of MLB pitchers to hit the mark has dropped from 34 in 2014 to 28 the next year, to just 15 each of the last two seasons. And 2014 was also the last and only year Strasburg hit the mark. But he’s averaged just 25 starts and 150 innings in the three years since, and has yet to clear 100 innings so far this year.
When Strasburg, who made his Nationals debut in 2010, was signed to a seven-year, $175-million extension in 2016, the prevailing wisdom was that the figure was some sort of discount. Strasburg may have been able to snag a higher value contract on the open market as a free agent. But that’s not necessarily the case, and considering he’s only been making about 75 percent of the available starts in any given season, he’s costing the Nationals an effective rate of basically $1 million per start.
As much as the Nats were publicly flogged for their conservative approach to Strasburg’s health, sticking to their self-imposed innings limit in 2012, his first full season back after his injury, their decisions in acquiring pitchers ever since has been far more aggressive.
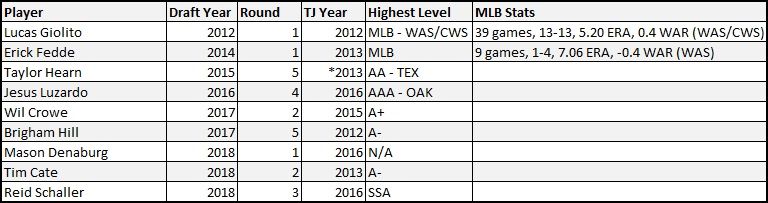
Since the 2012 draft, the Nationals have taken a high-risk, high-reward approach, regularly selecting pitchers who have already had Tommy John surgery. In the last seven drafts, they have taken nine pitchers with reconstructed elbows in the top five rounds of the selection process.
The trend began with Lucas Giolito who, with his 100 mph fastball and hammer curve, some speculated might be the first-ever right-handed high school pitcher selected No. 1 overall. He blew his arm out his senior spring. That didn’t deter Washington, which took him 18th overall.
Giolito never regained that full velocity, and his minor league numbers were mixed, right through his trade to the Chicago White Sox in the Adam Eaton deal. He’s 13-13 with a 5.20 ERA in 39 games (37 starts) so far in his Major League career (through Wednesday night).
The story of these draft classes has still largely yet to be written — the 2018 crew only turned pro in June. But plenty of pitchers drafted by other teams behind Giolito in 2012 have more accomplished MLB resumes. Michael Wacha (136 games, 32-32, 3.77 ERA) and Marcus Stroman (113 games, 41-33, 3.87 ERA) have been rotation mainstays for half a decade already. Jose Berrios made his first All-Star team this year. Not to mention Zach Eflin and Lance McCullers Jr. … that’s all before we even get to the second round.
Giolito and 2014 first-rounder Erick Fedde are the only two post-surgery pitchers the Nats have drafted in the first five rounds to have reached the big leagues, neither achieving stellar results. Only Jesus Luzardo, who was traded to Oakland in the Sean Doolittle deal last summer, is having any kind of success in the high minors. The landscape could change over the next few years, but thus far the draft strategy has not yielded the kind of results the front office clearly hoped it would.
***
When Strasburg hit the DL this June, it was for shoulder inflammation. In July of last year, it was for a nerve impingement in his elbow. In August 2016, it was elbow soreness. In June that year, it was an upper back strain. In July 2015, it was an oblique strain. That May, it was neck tightness.
“The arm is not a cannon sitting in a canoe,” said John. “If there’s any threat anywhere along that thread, that sequence of firing — anywhere — the whole system is suspect.”
As Yahoo baseball writer Jeff Passan concluded in his book “The Arm,” the only truly predictive factor when looking for a future arm injury is a past arm injury.
“But we can’t be so naive to say that an arm injury is just an arm issue,” said John, emphasizing that any breakdown along the kinetic chain can lead to a more catastrophic injury.
That’s why he starts taking injury history with the feet, the same approach that Dr. Annie Gow did when analyzing Justin Verlander as it appeared his career was slipping away in 2014. John doesn’t believe it’s a coincidence that Shohei Otani sprained his UCL this year three weeks after spraining his ankle.
While Douoguih doesn’t necessarily think any one injury portends another specific one, he sees the same issues as the body compensates for weakness.
“I wouldn’t say that there are predictable kinetic-chain injuries that occur, but you can see kinetic chain problems,” he said. “You can see stiffness in the shoulders the and hips that can lead up to it.”
***

While UCL reconstructions have become something of a specialty for him, Dr. Douoguih doesn’t want to perform any more than he has to.
“I remember some of the guys who didn’t get back,” he said. “Even in the best hands, sometimes they’re not able to get back to playing at the same level.”
He also understands that’s not always possible. He was encouraged by a report in the Orthopaedic Journal of Sports Medicine earlier this year, which showed promising return-to-play numbers. But having seen more of the long-term effects of the surgery over the last decade, he’s wary of the idea of investing in a player who hasn’t yet shown the ability to get back to his previous level.
“My whole thought process on that has evolved,” he said. “We didn’t have as much data seven or eight years ago as we have now. I, in general, like to be able to see that a guy has been able to get back to a certain level of play before we just pull the trigger and say, hey, let’s sign him.”
John wants more data before he makes his own conclusions about what to consider a successful recovery.
“Our measurement of success is so poor, because it just means that they came back and threw one pitch at their level of competition they did before,” he said. “I want to see numbers on who’s there three years, who’s there six years, who’s there 10 years?”
***

The cult of velocity is real. The Little League World Series, broadcast around the world on ESPN, not only shows the velocity that 10-, 11- and 12-year-olds are throwing, but how that compares, given the shorter distance between the rubber and home plate, to a Major League pitch.
Who wants to throw “an 85-mph fastball” when you could fire one up there “in the high 90s” instead?
At a recent showcase for 15-year-olds (itself a problematic scenario), a young pitcher looked down the bench and found three of his fellow participants wearing the elbow scar. For them to be back at full strength, at a showcase event, means it had been at least 12 to 18 months since they underwent surgery. That puts the time of the injury just above the age of those Little Leaguers you watched on TV this month.
These showcases, travel leagues, and the youth sports industrial complex in general have extended seasons into year-round endeavors. That’s more chances for injury, especially as wear and tear push young bodies to their limits.
“Every time you throw, you’re within 10 percent of the failure strain of the ulnar collateral ligament,” said Douoguih, who stressed that breaking balls and high-stress pitches only add to the chance of injury. “There’s a number of studies that show that overuse leads to injury later, or at least portends a worse prognosis in terms of injury later.”
Everyone can agree that it’s best to keep young arms as healthy as possible to try to prevent the need for surgery down the line, no matter how good the success rate is. But how do you keep young arms healthy in the first place?
***

Douoguih recommends limiting breaking balls before age 14 and avoiding two games in the same day. John similarly emphasizes not specializing in a specific sport until high school, limiting athletics to six months a year to give the body time to recover. More than anything, he said, you need a plan to combat the pressures of coaches and “experts” across the spectrum.
“All the decisions that are going to put your young athlete in the position to be their best self are going to be made in the home,” he said.
John’s new book is titled “Minimize Injury, Maximize Performance,” but it’s the subtitle that really drives home the treacherous reality of the youth sports landscape: “A sports parent’s survival guide.” His four-part process — Rethink, Replenish, Rebuild and Recover — focuses on building good core strength and nutrition for young athletes, taking the focus away from specialization and trying to bring the joy back to youth sports.
“It’s not fun anymore,” he said. “And youth sports are supposed to be a really good time. They’re supposed to develop them beyond just the physical. They teach teamwork and socializing (and) just how to have confidence in yourself as well.”
That starts with staying healthy. Even though Douoghui says UCL reconstruction is not a “death knell,” the more young players he can keep off the operating table, the better.
“A healthy arm without surgery, is something that I like to see — rather than with a scar on it — when they’re walking out onto the field at the Major League level,” he said.







