What’s known about expectant moms related to COVID-19 is changing every few weeks, according to a Northern Virginia physician who wants women to be extra-vigilant about preventing infection.
“This is called the novel coronavirus for a reason,” Dr. Alfred Khoury said. “Our information about it is very limited, and we are learning as we are going along.”
Khoury is the director of maternal-fetal medicine at Inova Fairfax and Inova Loudoun hospitals, and vice chair of obstetrics at Inova Fairfax.
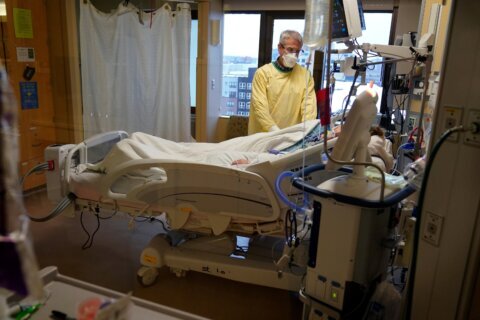
An unexpected development in pregnancies impacted by COVID-19 infection is that some women are more likely to be admitted into intensive care and put on a respirator.
Compared with women who are not pregnant, expectant moms with COVID-19:
- Have 1.7 times increased risk to be put on a respirator.
- Have 1.5 times increased risk to be admitted into the intensive care unit (ICU). “Absolute risk of being admitted to the ICU is 0.6% only. And the use of mechanical ventilation is only 0.2%,” Khoury said. “So, even though we are saying a lot of things that might be scary, the absolute risk is small.”
- ICU admissions are more frequent in pregnant women who were Asian, Hispanic or Latino and African American.
- But no data suggest an increased risk of dying.
Can expectant mothers infect unborn babies with COVID-19?
- There is a possible risk of transmission that is extremely small. “There is only one published clinical case that has confirmed a transmission of the COVID virus from the mother to the fetus while pregnant,” Khoury said.
Can COVID-19 cause abnormalities of baby development, such as with the Zika virus?
- No abnormalities have been seen associated with COVID-19.
- No increased risk of miscarriages has been seen in women developing COVID-19 during the first trimester.
Is there increased risk for stillbirth?
- A significantly higher chance of stillbirths has developed during the pandemic period, according to a just-released study from the United Kingdom: 9.31 stillbirths per 1,000 births during the pandemic, compared with 2.38 stillbirths per 1,000 births pre-pandemic.
- No increase in stillbirths was noted below 37 weeks. “Probably this is happening later than 37 weeks,” Khoury said. (Most pregnancies last around 40 weeks.)
While stating that the stillbirth information is reflected only in one paper that was released in just the last few weeks, Khoury still wants expectant moms to carefully monitor their conditions.
“My recommendation to patients is to be very diligent in watching the kick counts, making sure the baby is moving, talking to the doctor about how to monitor themselves after 37 weeks if they have COVID-19.”
Is there an increased risk for pre-term births?
- Pre-term birth increases have been reported among COVID patients, but it’s unclear whether that’s secondary to the virus, or secondary to patients and doctors reacting to the disease by deciding to deliver earlier.
“This is what we call iatrogenic delivery and probably not due to spontaneous pre-term labor,” Khoury said.
COVID-19 infections alter the birth experience and impact the baby-mom bonding relationship and nursing.
Khoury said skin-to-skin contact is more difficult, and that mothers have to take extra precautions such as frequent hand washing and wearing a mask while nursing to avoid infecting their infants.
Babies born to virus-infected moms are treated as though they have tested positive and are separated in the nursery.
Khoury recommends the following sources of information for expectant mothers:
American College of Obstetricians and Gynecologists
Society of Maternal-Fetal Medicine
California Maternal Quality Care Collaborative
- Sign up for WTOP alerts
- Latest coronavirus test results in DC, Maryland and Virginia
- Hogan overturns Montgomery County closure of non-public schools
- ‘Too many are selfish’: US nears 5 million virus cases
- Progress ‘long ways away’ as urgency grows on virus relief
- Historians draw comparisons between victims of 1918 H1N1 pandemic, modern coronavirus
Looking for more information? D.C., Maryland and Virginia are each releasing more data every day. Visit their official sites here: Virginia | Maryland | D.C.