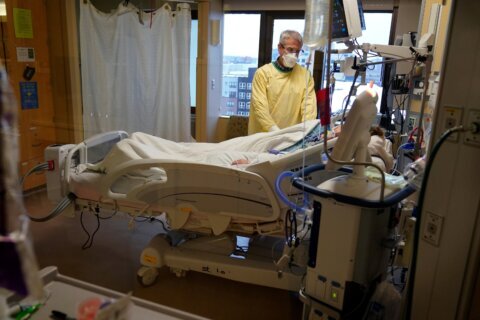
For those on the front lines of the fight against the coronavirus, the pandemic has provided many unexpected hurdles and that was no exception for those caring for the sick in hospitals.
Dr. Peter Olivieri, a pulmonary and critical care physician at the University of Maryland Baltimore Washington Medical Center, said responding to the unknown was a struggle at the beginning of the pandemic.
“That creates a lot of challenges both psychologically for the patients and families, as well as the health care providers and also just medically since we really didn’t have any treatments for the condition,” Olivieri said.
For health teams, it overcame initial fears about their own safety as they helped patients fight an unknown disease.
“A lot of it has just been getting the experience with seeing so many of these patients and getting a feel for what the clinical course looks like,” he said.
Olivieri said nurses, doctors and other members of care teams had to quickly adapt wearing N95 masks and other more specialized protective face coverings, including powered air-purifying respirators while doing their jobs.
“These are things that we would previously have only maybe used a few times a year for things like tuberculosis, and now we’ve gotten into a groove where we’re essentially using these things multiple times every single day for months in a row,” Olivieri said.
Unlike other respiratory diseases he has helped treat in the past, the time some people spend on a ventilator with COVID-19 was surprising for Olivieri.
“They’re not just mild cases, where they may require life support for 24 to 48 hours and then come off the breathing machine. These are on the more severe end of the spectrum, such that they are requiring life-support, in some cases, for weeks,” he said.
Olivieri said hospitals also had to learn to adapt quickly to make room for patients. At his hospital, that included temporarily expanding the intensive care unit.
Another major struggle was helping patients stay connected with their loved ones who could not visit them.
“We’re used to having those family members there as part of the team,” Olivieri said.
Looking back at the first few months of the pandemic, Olivieri said there are lessons learned for the health care industry, including stocking up even more on supplies, such as protective gear for these types of situations.
“I think that there’s definitely a lot of room for improvement in terms of being prepared for the next wave, whether it’s this particular disease or the next emerging infectious disease,” Olivieri said.
He said health care teams rose and continue to rise to the challenge at his hospital, where 80% of the most severe patients recovered from the disease and went home.
- Sign up for WTOP alerts
- Latest coronavirus test results in DC, Maryland and Virginia
- Coronavirus FAQ: What you need to know
- Coronavirus resources: Get and give help in DC, Maryland and Virginia
- Montgomery Co. restaurant that defied mask requirement likely to change ownership
- Silver Spring man feeds thousands of neighbors during the pandemic
- Socially distanced tables, $100 cabanas in Hook Hall’s back yard
Looking for more information? D.C., Maryland and Virginia are each releasing more data every day. Visit their official sites here: Virginia | Maryland | D.C.