Debates are raging across the United States on the best ways to handle the coronavirus pandemic and many people have entrenched themselves in one camp or another — often drawn along political lines.
WTOP’s John Domen spoke with Dr. Martin Makary, a surgical oncologist and chief of the Johns Hopkins Islet Transplant Center, about the importance of facing the pandemic and the conversation surrounding it with nuance.
Read their full conversation below:
A lot of people are afraid of breakthrough infections after being vaccinated — what do these breakthrough infections tell us about the effectiveness of the vaccine?
I think there’s a feeling that a breakthrough infection represents a failure of the vaccine, when in fact, it really represents the success of the vaccine in reducing a serious illness to a mild common cold, like illness or asymptomatic case. You know, there’s a perception out there that the vaccine was going to really eradicate COVID, or create a force field around somebody like a bug zapper almost. And the reality is that people need to recognize that we’re downgrading COVID from a major public health threat to a mild manageable illness that will probably be seasonal and endemic for a long time.
How do we get to a place where we’re not as scared of the virus?
I think we have to recognize that a positive test is not an indication of a major problem, if it’s in the context of people who are immune. And there’s a lot of people out there who are immune. for example, the Olympic athletes are the lowest risk people for COVID on planet Earth — they’re healthy, they’re young, they’re all fully vaccinated. And yet, when they had an asymptomatic positive test result, they [were] disqualified, that sends the wrong message. What we need to do is focus all of our efforts on specifically non-immune adults, those are the people dying at a high rate right now.
How concerned should parents be for their children who are too young to get vaccinated?
For the last few months, there have been more children in the hospital with [respiratory syncytial virus] than with COVID-19. I’m not downplaying COVID and kids — but people need to understand the risk, and I think people have a distorted perception of risk. The risk in children is incredibly skewed towards those with a pre-existing condition. And for those kids, they really want to take all precautions, but we need to recognize that the case fatality rate is comparable to seasonal flu, we’re seeing a lot more COVID.
About half of kids have had COVID — and we need to do everything we can during an active outbreak — but the idea that we need to take a hit on their livelihoods, on being there in person, on their activity level, those are things that we need to weigh the risks and benefits because we are seeing consequences of the mitigation in children, like we did last year.
You’ve taken a sort of nuanced, maybe middle ground approach, on vaccines. You’re clearly for them — you’ve made that definitely clear — but that mandating them for “every living waking American” is maybe a step too far. Can you elaborate a little bit about that? And how do children fit into that?
There’s a lot of people who say “I had COVID, I was sick and recovered. I don’t feel that I need the vaccine.” And right now the science is on their side. Now that could change, but we’ve got a good year-and-a-half of observational data on people who had the infection. We do not see reinfections cause severe illness, and when they happen they are infinitesimally rare. Turns out, the natural immunity from prior infection is 27 times more effective than vaccines in preventing symptomatic COVID. Now, I think a lot of us have been afraid to talk about this and public health officials have not been recognizing it because it’s a nuanced thing. And because you don’t want people to go out there and deliberately get the infection to try to get that immunity. We want people to get vaccinated instead, because it’s a much lower risk path. You don’t want to risk the consequences of COVID.
So it’s nuanced, and the country doesn’t do nuance very well. So we’ve had an indiscriminate blanket vaccine policy for everybody. The reality is if you’ve had COVID infection, you’ve got immunity and you can get one dose — that’s what many of us recommend.
With children, it’s important to know that natural manner is effective because the second dose of the vaccine and teenage boys can have a risk of heart complication, rates that exceed the risk of hospitalization from COVID.
So can we quantify exactly how good natural immunity is compared to the vaccines? And what do we know about how long natural immunity lasts?
We have the observational data of about 19 months, coming on 20 months, where worldwide, physicians have had the observation that people do not get reinfected with severe illness, we just don’t see it. And by the way, the other coronaviruses that cause severe illness in humans — SARS and MERS — also give long-lasting immunity. So it’s not that big of a jump from the other coronaviruses that cause severe illness. But we do see the activation of B and T cells, which tells us in general, that the immunity is long-lasting, that was the data out of the out of Washington University.
Cleveland Clinic looked at 1,300 health care workers, six and eight months after they had COVID. And guess what? Zero got reinfected. Now another big study looked at a quarter million people who had COVID and about 234 tested positive, but mostly asymptomatic. So the data are pretty compelling that natural immunity is effective, but it’s just something to factor when we talk about vaccines. It just allows us to be more precise when we say these are the people who really need to get vaccinated. If you just look at who’s dying in the hospital right now, the vast majority — 99% — are adults who have no natural immunity and no vaccinated immunity. That’s where all of our efforts should be focused right now: on saving lives.
Do we know how long natural immunity would show up in testing? I had what would be considered symptoms at the start of this, before we realized that it was even something over here. I’ve since received the vaccine. Is there a way to tell whether or not there was some natural immunity there? How do people know how much immunity they might have?
Many laboratories will offer the basic test to find out if you’ve got antibodies, and they’ll actually be able to distinguish if it’s ordered properly. Whether or not you have antibodies to the infection or to the vaccine, we can tell the difference. And right now those people who have not had COVID infection are eligible for a study that we just announced yesterday … studying natural immunity, but people can go and get tested for this and know their status.
Now, the antibodies don’t tell the full story because they come and go, we’ve always known that’s true with any infection. But usually you can detect it up to six months to a year, and sometimes longer. But the B and T cells are activated and those are harder to measure. We don’t have a very good, reliable test for that what we call cellular immunity. Those are sort of the tanks in the warfare against the virus. [They are ] slower to mobilize, maybe a few days, but they’re very effective. And that’s why we believe immunity is long lasting, and many people who had the infection.
If you were one of those advising President Biden right now, what approach would you to living with and working around everything right now?
I would say that we need to stop the arguments over cloth masks and three-year-olds; stop the arguments over boosters and young people and focus all of our efforts on the non-immune adults through sharing testimonials. We don’t need more celebrities or politicians running ads. We need testimonials out there.
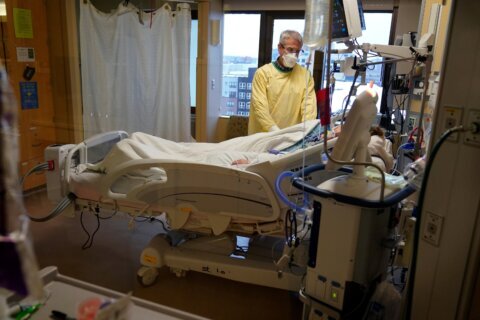
I know of people who have physicians who have had patients come in … seconds before they get intubated — and by the way, that’s one of the worst feelings anybody can have is not being able to breathe — they asked for the vaccine. Well, it’s too late. We need to share those stories out there. As COVID illness is becoming relatable, we’re seeing more people go out and get the vaccine.
I would also tell people, the dosing interval that is between the first and second Pfizer and Moderna vaccines should really be three months or six months, not three or four weeks. It’s very obvious from the data, from experience with other vaccines, that that three to four week interval is too narrow, and the only reason we’ve stuck with it is because of the rigid FDA regulatory process where they put out something and really never revise it. The data are overwhelming that your immunity is stronger, better. If you get that second dose, a good three months or more out. And if you do so, as I did for myself, you probably will never need a booster.
So does that mean some of the things we’re doing in schools right now, with the testing and the masking, are you suggesting — I’ve got a four year old who has to wear a mask to preschool every day, is that sort of unnecessary? Or am I reading you wrong?
You know, there’s no good solution for schools, there’s really no good solution. This epidemic is becoming endemic, and it’s ripping through schools, and you’ve got schools, for example, Palm Beach County, they do absolutely everything that we asked them to do. They have everybody with universal masking, distance, ventilation, teacher vaccination, and guess what it rips through that school. So it’s almost as if, regardless of what’s done, it still is spreading in a way that’s uncontrolled in that younger population that’s not vaccinated. So there’s no good solution. I tell folks, we still got to do everything during an active outbreak. Let the schools decide what they believe to be the best strategy. And for those schools that ask for my opinion, I tell them do everything for now. By the way, the quality of the surgical mask matters, the cloth mask is probably close to ineffective, at least in the cluster, randomized control trial. A surgical mask does help but it’s an 11% reduction in transmission, not a big benefit. N-95’s are better. But remember, the masks we’ve assumed have no harm. And that’s not true. Some kids do well with masks. Matter of fact, most. But some kids really struggle. And those struggles can be profound, and kids with disabilities learning, cognitive hearing loss, and we’ve got to have carve outs for those situations.
What would you establish as the right exit criteria, and what’s the off-ramp to trying to get back to normal?
Ten cases per 100,000 is the threshold — once crossed, I think people should be back to normal and those who are not vaccinated as adults without natural or vaccinated immunity have made a poor decision, but they do so at their own individual risk. The idea that they pose a public health threat to those vaccinated is really just a threat limited to a mild common cold or asymptomatic infection.
We would never have these massive culture wars over the flu. We would never say the unvaccinated from influenza pose a public health threat to those vaccinated from influenza. At some point we’ve got to recognize that we’ve got to move on and live our lives — there are consequences of restrictions. We’re polarizing the country around areas where we should have broad consensus. And we shouldn’t be divided over who’s legitimate and who’s not legitimate in their ability to work and thrive. Everybody is an essential worker, in my opinion.
What frustrates you the most about the response to the pandemic, and what do you think needs to change?
I think we’ve seen tribalism in the United States polarize us over this issue of COVID-19. And we’ve seen it in the medical profession. There’s a lot of groupthink, and there has been for a long time.
If you look at the issues I’ve written about in the past on the lack of appreciation that food is medicine, and that we need to start addressing lifestyle changes and researching environmental exposures that cause cancer, not just chemotherapy, there’s been a lot of groupthink in medicine.
With COVID, we got burned because we basically followed a small group of people who had a uniform opinion. And that opinion was evolving, and it has not been correct or optimal for much of the strategy. For example, when we had the vaccine, we dealt with tremendous regulatory burdens … as 1000s of people were dying a day. Then we got a very rigid recommendation that the first two doses of the vaccine have to be three and four weeks apart — we should have spaced it out to three months, we didn’t see that flexibility. Then we recognize natural immunity data was an incredibly powerful, and we should have. And we should have acknowledged natural immunity. But we didn’t. And as a result, tens of thousands of Americans died, because we gave the vaccine early on to people already immune when we should have had them step aside in line to save vulnerable Americans.
We’re in a situation where we know that second dose should be spaced out to three months, and we’re not seeing the flexibility or the recognition of natural immunity.
So we have had too rigid of an old guard medical establishment groupthink on so many of the key issues, when many of us have put out different opinions respectfully, and it’s been relegated to ‘Oh, but the CDC says this,’ or ‘Oh, but Dr. Fauci says this.’ Fauci is a wonderful human being; I respect him a tremendous amount, but he’s also one medical opinion. And that opinion has dominated public discourse, when really there have been other opinions that we needed to hear that we did not hear through much of the pandemic.