Vanessa Strunk is a self-described “boring old lady” who goes to work, shops online and heads home at the end of the day.
A small business owner who runs the Rockville, Maryland-based Green Diva Designs firm, the 58-year-old said she had been taking precautions since the coronavirus pandemic hit in March.
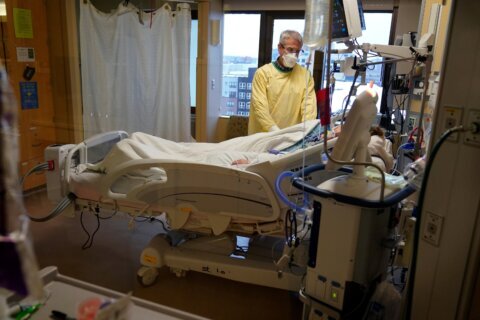
But she never expected to be in a local intensive care unit hearing a doctor tell her that they were doing all they could — but that they were hitting the limits of what medicine alone could do.
“I knew at that moment, either I’m going to live or I’m going to die,” Strunk said.
The beginning
It started in mid-November, when she struggled to get out of bed one morning.
“It felt like kind of the flu,” but different.
Strunk felt “extreme exhaustion getting out of the bed and moving around.” Just getting to the bathroom took incredible effort, she said.
Right away, she thought it could be COVID-19. She wanted to get things squared away in case she ended up in the hospital.
Strunk arranged to get tested. A planner by nature, she said, “I had no idea what was coming for me.”
Her COVID-19 test was positive. She arranged to quarantine, expecting and hoping to ride it out on her own at home.
By Nov. 19, her condition worsened, and she went to MedStar Montgomery Medical Center in Olney, Maryland. At that point, she didn’t meet the criteria for admission, so she was sent home.
Strunk bought a medical device on Amazon that measures your oxygen levels. She watched with growing alarm as the numbers showed her oxygen levels dropping as her condition worsened.
‘I couldn’t breathe’
On Nov. 21, she went back to the emergency room at MedStar Montgomery and was admitted.
First, she was on a medical-surgical floor. As she needed more care, she was taken to a step-down unit where patients go when they come out of the intensive care unit.
Then things shifted. “I was declining. I couldn’t breathe. So they took me to the ICU,” Strunk said.
Dr. Manu Kaushal was part of the team coordinating Strunk’s care. Kaushal, a pulmonologist, is the medical director of the ICU at MedStar Montgomery.
Every time he enters the room of a COVID patient, Kaushal told WTOP that he pauses for a moment.
Kaushal said he knows he’ll be asked what the outlook is, and he wants to strike a balance between offering comfort and being honest.
“When I go in, I am not sure if this patient is going to make it, or of how long the battle is going to be,” he said.
Although she was exhausted and on medication, including anxiety medication, Strunk’s memory of one moment is crystal clear.
Strunk said Kaushal told her, “You have a 50/50 chance — fight.”
Kaushal said Strunk’s recollection of his words was accurate.
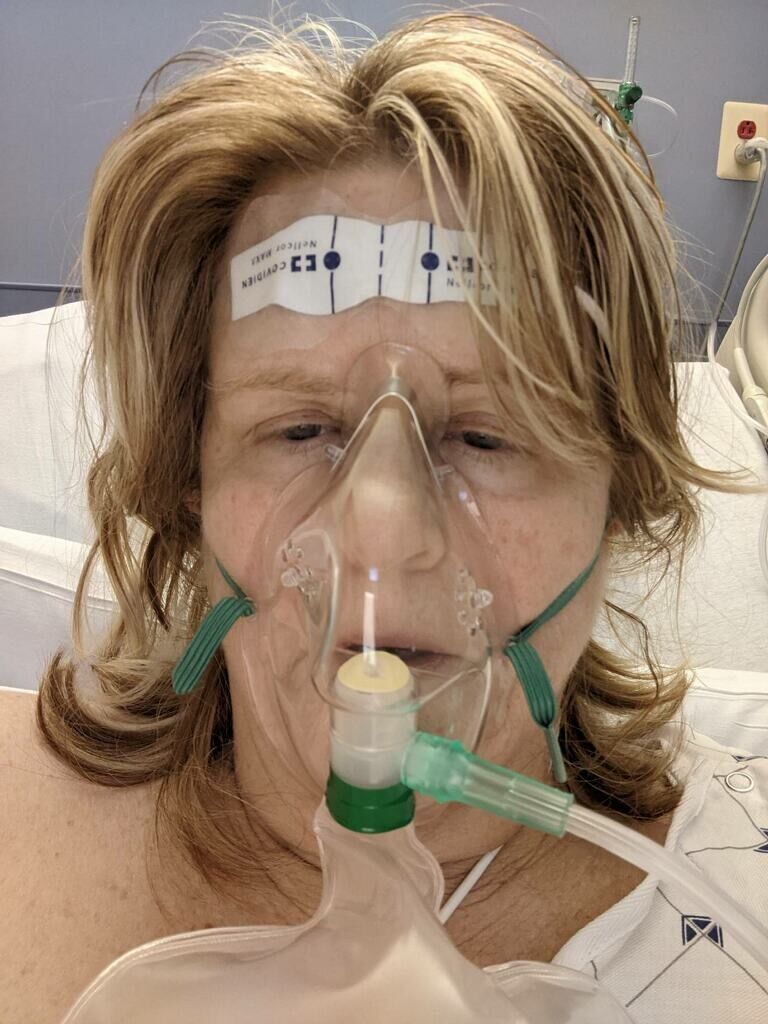
He explained that Strunk was receiving 60 liters of oxygen per minute.
A typical non-COVID-19 patient in need of oxygen would get two, four or six liters — maximum. Strunk was getting 10 times that amount.
“Once they get into the ICU on that much oxygen,” Kaushal said, “it’s anybody’s guess which way this is going to go.”
Fighting with the disease, not against it
Speaking to WTOP from her hospital bed one day, before being told she would likely be going home, Strunk said, “The ultimate thing that has changed my life is looking into the eyes of a doctor who you know is doing everything he can, who’s being 100% honest with you,” and hearing that doctor say that the medical team had done everything they could, but that she would have to wait to see how the virus would respond.
Strunk said she had a pep talk with herself at that moment, saying, “Let’s see what happens. I’m gonna fight.”
But she told WTOP that what she learned was she would have to fight with the disease, not against it.
Anxiety, doctors explained, is the enemy.
Dr. Ramani Reddy, an infectious disease specialist at MedStar Montgomery and part of Strunk’s care team, explained that because patients can’t have visitors and must be isolated, their understandable concern can spiral into fear. Reddy said doctors have to take on the role that family members often fill.
She described frequent visits to hold Strunk’s hand and telling her, “Hang in there. you’re getting there, you’re getting there.”
Strunk recalled that “you’re just supposed to lay there and wait, and try to breathe and try not to panic.” So she would think to herself, “Come on, body, we can do it. Relax. Breathe.”
Kaushal explained that the level of oxygen being pushed into a COVID patient’s airwaves can actually exacerbate the sensation of not being able to breathe, even though the process helps deliver critically needed oxygen.
Panic is dangerous, Kaushal said, “because this will lead you to breathe much faster, which can drop your oxygen levels even further.” If that continues, he said, it can lead to what every doctor who treats COVID tries to avoid: having to put a patient on a ventilator.

Turning the corner
Strunk was fortunate. As suddenly as she declined, she began to turn a corner.
Reddy vividly remembered the day the turnaround was evident. When she walked into Strunk’s room, her patient was no longer prone, but sitting up in bed, smiling broadly.
“It was such a good feeling to walk in and see her smiling and not needing any oxygen and able to talk without stopping and gasping to catch her breath,” Reddy said.
“And then she started crying,” Reddy said.
The tears were tears of joy. And gratitude.
“They’re saints and angels,” Strunk said of her doctors, nurses and the health care support staff.
“They do it because that’s who they are. But still, they’re human beings. And they’re exhausted, and they’re suffering themselves.”
The mental toll
Kaushal said Strunk is right — health care professionals, who are facing increased patient loads and seeing critical care beds fill up, are feeling the effects of caring for so many seriously ill patients, one after the other.
“You know, the burnout that the health care workers are experiencing at this time is absolutely beyond imagination,” he said.
When asked about the toll of dealing with COVID patients, Reddy said it was worse at the start of the pandemic, when so much about the erratic disease was unknown. “Especially back in beginning when we started in March and April, there were days I came home and would cry.”
There was a frequent and unfamiliar sense of helplessness, according to Reddy. “You want to do something, but you don’t know what else to do.”
Doctors as family
Often the only thing doctors can do is be there for patients when family members can’t, Kaushal said.
He said of patients in the ICU who don’t make it: “We are actually holding their hands as they take their last breaths.”
Kaushal added that he will often “huddle up” with staff and they’ll exchange positive stories to keep each other’s spirits up.
“I come home and talk to my daughter and my husband. That’s what makes my day better,” Reddy said.
Importance of basic safety measures
Both Kaushal and Reddy said that while vaccines are being introduced and distributed in phases, the need for basic precautions continues.
“We know the most effective treatment for this thing is prevention,” Kaushal said. “That’s the best treatment.”
He added: “We know masks work.”
Kaushal and Reddy both hope that people continue to wear their masks, and that those who remain skeptical will change their behaviors.
“Trust me, when I see sometimes people in grocery stores with their mask on their chin, I want to go to them and tell please pull it up,” Reddy said with a laugh.
Strunk, now at home, said she decided to share her story because she wants to make people understand the reality — and the severity — of COVID-19.
Still breathy when she speaks, and now being observed as a possible “long hauler” COVID case, Strunk said she understands the desire to socialize, especially during the holidays. But she’s adamant that people should stay at home.
“You don’t realize what you have at stake,” she said.
Kaushal’s prescription in the meantime is simple: “Masks, social distancing and hygiene — simple things.”
If everyone does their part, he said, “We can get over this thing.”
EDITOR’S NOTE: WTOP reporter Kate Ryan previously hired Vanessa Strunk’s firm to do some renovations on her home 15 years ago.