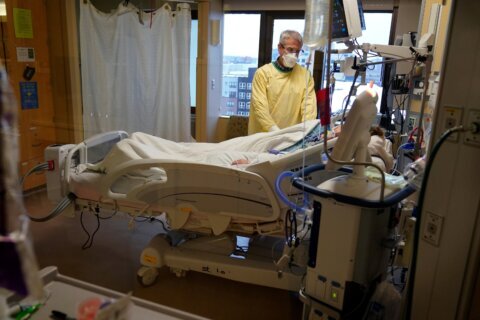
As the nurse manager in the intensive care unit at Shady Grove Medical Center, Nimeet Kapoor is used to spending a lot of hours tending to patients with a lot of infectious diseases. But the illness and the deaths brought on by COVID-19, he told WTOP, are something else.
He said it means 10- to 12-hour shifts in a unit with 49 beds that usually has 28; it means a lot of “learning as we go,” and it means a lot of time on the phone with people whose loved ones might be slipping away.
“No school, no books, no education prepares you for what we’re going through right now,” Kapoor said.
‘The fear is also real’
Very sick people in an ICU is nothing new, “But these patients get sick very fast,” Kapoor said. “And they don’t have that many other problems — they strictly have respiratory ailments” from COVID-19.
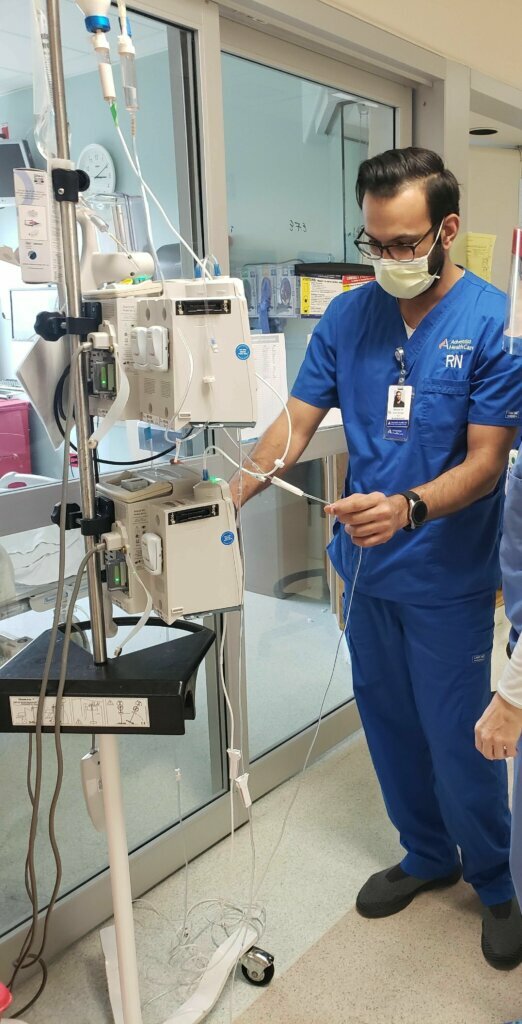
And while they’re used to dealing with infectious diseases, the nature and the newness of the virus mean there’s still a lot they don’t know — and that’s a worry.
“We are used to seeing a lot of infectious diseases on the floor that we gear up for,” and COVID-19 is no exception, he said.
On the other hand, “The fear is also real; I wouldn’t lie — the fear is in the back of the mind. But when it comes to the day-to-day activity, it’s just like any other patient.”
Kapoor said he spends a lot of time on the phone with families of patients, since the nature of COVID-19 means they aren’t able to spend time with their afflicted loved ones.
“The families are having a difficult time with it. Some families understand that there’s a pandemic going on and some don’t,” Kapoor said, adding that he understands. “I feel like if it was my loved one, I would want to be close to them as well.”
At Adventist Healthcare, being a faith-based organization, chaplain services are heavily involved with patients, including in their final moments.
“The nurses, the doctors are usually at bedside during the final moments as well. If it was my loved one passing away, I would want someone to be with them holding their hand to mitigate the situation as much as possible,” Kapoor said.
It’s a scene Kapoor has seen quite a bit recently, and he said when a patient dies, everyone around the bed takes a pause.
“What we do is, we recognize the patient. The chaplain services make the prayer right after, and then we recognize the person and the hard work that we put into it. And then we take a pause for about 15 seconds and then we walk away from it.”
He said the chaplains help the medical staff as much as they do the patients.
“As health care providers, sometimes we get immune to people passing away around us,” Kapoor said; chaplain services “bring us back to reality. … To, I don’t know, make us believe that we are humans too, and it’s OK to be emotional about it and to recognize those emotions.”
All they can do is look out for each other: “We’re doing a lot of checks on each other,” reminding each other “We will get out of this on the other end. … It’s definitely learning as we go and preparing for what’s coming.”
That said, “It definitely is taking a toll,” Kapoor said. “I won’t lie. It’s taken a toll on a lot of us.”
‘We have what we need right now’
As to how close to that “other end” the region is, Kapoor is guardedly optimistic.
“I think we are toward the top — we are definitely not going toward the bottom of the hill,” He said. “We are either at the top or near the top.”
While hospitals in places such as New York were running out of masks, gowns and gloves — the personal protective equipment, or PPE, that has become a common term in 2020 — Kapoor said the situation in his hospital was not great, but could be worse. Each nurse gets one mask per shift and discards it at the end of the day. “We have what we need right now,” he said. “I think if we had more, that would be better.”
- Sign up for WTOP alerts
- Popularity of Maryland-themed masks helps buoy Towson business
- Quarantine art highlights well-known DC spots, profits go to charity
- Virginians stuck at home are fed up with noise from Amazon headquarters project
- Latest coronavirus test results in DC, Maryland and Virginia
- Coronavirus FAQ: What you need to know
- Coronavirus resources: Get and give help in DC, Maryland and Virginia
For a lot of people in the D.C. area, putting on gloves and a mask is a new experience — often a hot, uncomfortable, glasses-fogging experience. But like anything, do it enough times and it becomes part of the routine.
Once the gown and mask and gloves are on, “It is uncomfortable in the beginning,” Kapoor said. “You are definitely drenched in sweat, but once you’ve been in there for about a half an hour, you get used to it. … When you take it off, you realize you’ve had it on for a long time.”
The key to prevention
Asked what people can do to make his work easier, Kapoor’s answer wasn’t exactly groundbreaking: social distancing, wearing a mask and washing your hands. It’s not new advice, but it works.
“That is the key to preventing the spread of the virus,” Kapoor said. “As a nurse, I‘ve been saying this for years. I promote that to my own family members. And they listen, and they don’t listen sometimes.”
He emphasizes again that even for an experienced nurse, this is new territory.
“I did not imagine ever in my life that I’d be doing something remotely close to this, or seeing our society where it’s at right now. But this is a crisis, and we’re doing the best we can to get through it.”
WTOP’s Dimitri Sotis contributed to this report.