WASHINGTON — First, it starts with a sore throat. A fever, a headache and swollen lymph nodes likely follow. And for most living in the U.S., a prescription for antibiotics isn’t far behind.
But for patients living in low-income countries with limited access to care, it’s not uncommon for strep throat to go undiagnosed. And when it does, it can lead to serious problems, including a type of heart disease that’s responsible for more than 300,000 deaths each year.
“As the body is trying to fight the sore throat, it ends up attacking the heart and leads to a long-term heart valve problem, called rheumatic heart disease,” explained Dr. Craig Sable, associate chief of cardiology at Children’s National Health System.
On Nov. 24, Sable and 10 doctors, nurses and health care professionals from Children’s National boarded a 13-plus-hour flight from Dulles International Airport to Uganda to perform surgery on seven children living with rheumatic heart disease (RHD) and four others diagnosed with congenital heart disease, ranging in age from four months to 21 years old. It was Sable’s 13th surgical mission to the East African country, where RHD is the most common cause of heart disease in young adults.





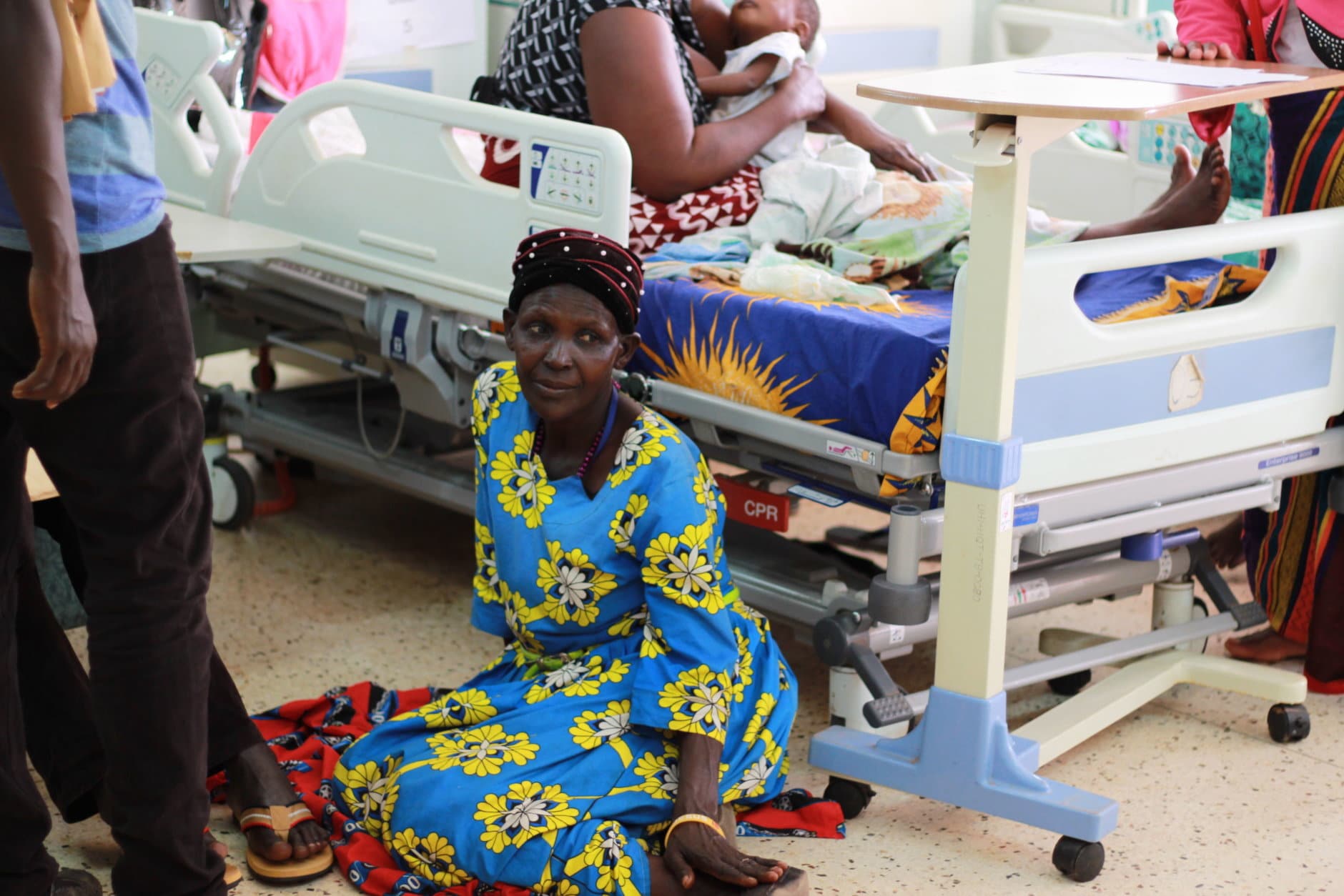









“Many of these children are severely limited. They have swelling in their abdomen, they have extra fluid in the their lungs, they have trouble breathing; many of them can’t go to school,” said Sable, who partners with the Uganda Heart Institute for the surgeries.
With treatment, however, life can return to a more normal state. Just two days after 12-year-old Deng Daniel’s 12-hour open-heart surgery, Children’s National nurse Erin Esposito Shand said the patient was “playing basketball” from his bed, using her arms as a hoop.
“Anybody who works here can all say that pediatric patients recover and do much better than adults do, at baseline, but the resilience that you see with the patients in Uganda is like nothing I’ve experienced before. And I think what’s unique is it’s not just the patients, it’s their families,” said Shand, who added that many families traveled long distances to make the surgeries and slept outside the hospital on straw mats while their children waited for their procedures.
Sable has been working with doctors and nurses in Uganda since 2003, and over the last 15 years, the focus of his work has shifted from purely patient care to include training and education for the medical staff in Uganda. With each trip, Sable and Children’s National surgeon Dr. Pranava Sinha pick a new procedure to teach the doctors, nurses and staff at the clinic in Kampala. When they leave, the Ugandan team continues on with the new surgical specialties.
“In Uganda, as in many low-income countries, these children live in villages where 20, 30, 50 people are taking care of them, so fixing one kid impacts dozens of people,” Sable said.
“But on the macro level, we’re trying to develop a sustainable program where Ugandans can take care of patients, themselves. And so hopefully every surgery we do there, that leads to another 10 or 15 children that can be helped by the Ugandans.”
Using funding from grants and donors, the Children’s National team also arrives with supplies and resources that the clinic may otherwise lack. Sable has also conducted RHD screenings and even set up telemedicine clinics in some of Uganda’s rural villages as a way to improve access to care.
Sable said the Uganda Heart Institute is now able to treat about 200 patients a year. But still, more needs to be done — in Uganda and beyond.
While rare in the U.S. and Europe, data from Children’s National show that more than 33 million people are living with RHD, and 80 percent of the world’s children live in areas where RHD is endemic.
“The impact of rheumatic heart disease is on the same magnitude as HIV, [tuberculosis], and malaria and a lot of other diseases that people think about as being really important,” Sable said.
“The fact that rheumatic heart disease gets very little attention has resulted in minimal funding for research and advocacy to ultimately lead to prevention and eradication.”
But until more efforts and money are funneled into RHD research, Sable and his team from Children’s National will keep working to change the lives of Ugandan children, one patient and one physician at a time.
“Every child that we’re able to touch and every family that we’re able to give the gift of their daughter or son being able to come home and be healthy is incredible,” he said.