A naloxone nasal spray should be sold over-the-counter, a panel of the Food and Drug Administration’s outside advisers unanimously voted Wednesday, clearing the way for the regulator to broaden access to reversing drug overdoses.
The spray works by temporarily reversing the effects of opioids, ranging from prescription painkillers to heroin to fentanyl. When administered soon after an overdose, it can avoid brain damage and death until paramedics arrive.
The vote follows a daylong joint meeting of two FDA advisory panels to weigh a request by Emergent BioSolutions, the manufacturer of Narcan, to sell the product over the counter.
Approving nonprescription use of naloxone could allow the spray to be distributed everywhere from vending machines to bigbox stores, the FDA said. Online ordering might also be an option, the company told the panel.
“Over seven years of having marketed this product, we know that this product is very easy to use. It is being used by a variety of community groups, including lay individuals. It is a single four milligram dose that is safe and effective,” Manish Vyas of Emergent BioSolutions told the committees.
Emergent said in a statement that it was “premature to discuss” details of how much its drug-device combo would cost. The over-the-counter version could be available as soon as this summer, the company says, once production ramps up after approval.
Naloxone costs can average as much as $250 for uninsured Americans, though insurance and other nonprofit or local government programs often offer subsidized or free options. The company said it is working with retailers and government officials on plans to distribute it.
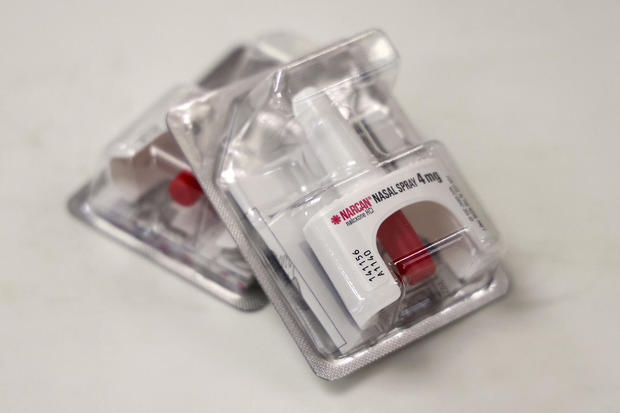 Two doses of Narcan, which can be given for a opioid overdose in an emergency situation.
Two doses of Narcan, which can be given for a opioid overdose in an emergency situation.
Terrence Antonio James/Chicago Tribune/Tribune News Service via Getty Images
Another over-the-counter request for naloxone from nonprofit Harm Reduction Therapeutics, for its RiVive product, is also scheduled to go before the committee next month.
Naloxone has already been available for so-called “community” distribution to reverse overdoses since 2016, allowing many to administer the potentially life-saving spray immediately before attempting to reach 911.
Most states have standing orders or similar measures allowing pharmacies and other organizations to dispense naloxone without patient-specific prescriptions, as well as “good samaritan” laws to protect bystanders who intervene in overdoses.
But health officials and outside groups say many Americans still face barriers getting naloxone.
“We have heard from stakeholders, including harm reduction groups, that some pharmacies are reluctant to carry naloxone or find the standing orders burdensome,” the FDA’s Dr. Jody Green told the committee.
The FDA announced in 2019 it would take a further “unprecedented” step of developing its own labeling – initial steps typically left up to drugmakers to pay for – in hopes of encouraging manufacturers to pursue selling naloxone over-the-counter.
“Additionally, for some who use opioids, the stigma of opioid dependence may inhibit purchase requiring an interaction with a pharmacist. We believe that non-prescription naloxone may help address these barriers,” said Green.
Emergent adapted the FDA’s model labeling for Narcan. The company ran its own validation study to simulate people using the spray while following their directions.
However, FDA officials told the panel that they had identified a handful of shortcomings with the company’s study. And despite limitations that may have biased the study towards positive results, the regulator noted there were still errors using the spray. Some users started on the wrong steps or administered the spray incorrectly.
The FDA and Emergent said they were still in talks over the final label, which is among other issues – like around manufacturing – that still need to be resolved.
Advisers on Wednesday wrestled over a handful of discussion questions over tweaks that might reduce the risk of errors, including the lack of research on how easily children can navigate the instructions.
“To not have specific studies to help really hone in on how to make the instructions readable to them is a failing of us in trying to develop things,” said committee member Dr. Leslie Walker-Harding.
“I do not think we need to wait with this, because every day we wait there are more people who are going to die,” she added.
The regulator is expected to issue its ultimate decision over Narcan by March 29.







