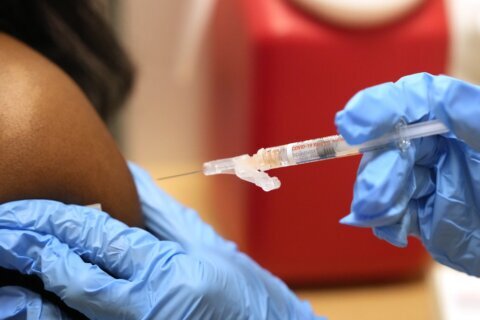
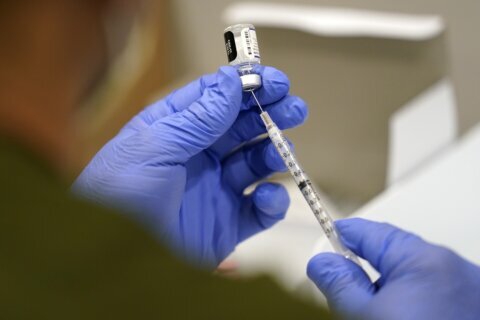
▶ Watch Video: Biden aims for 70% of American adults to have at least one COVID shot by July 4
While the Biden administration has been racing to maximize the number of Americans vaccinated against COVID-19, government researchers have also been working on what form the next generation of vaccines will take.
They may be combined with the seasonal flu vaccine, or could come in the form of pills or patches instead of shots. Scientists also envision vaccines that might shield against viruses beyond SARS-CoV-2 (the virus that causes COVID-19) that could avert future pandemics.
And they’re evaluating whether those who are fully vaccinated might need booster shots later this year. Additional shots could be virtually identical to the first doses, given as a safeguard against the possibility of waning immunity or tweaked to defend against mutant strains that are raising concerns.
Here’s what we know about the next-generation landscape of coronavirus vaccines:
Booster shots
The three major vaccine manufacturers with shots authorized in the U.S., Pfizer, Moderna, and Johnson & Johnson, have plans for — or are already testing — an additional shot. The booster shots are expected to be very similar to current vaccines but could come in a smaller dose.
“With many vaccines, we understand that at a certain point in time we need to boost, whether that’s 9 months, 12 months. And we are preparing for that,” Dr. David Kessler, chief science officer for the administration’s COVID-19 response, told lawmakers last month.
Boosters might also be blended with the annual seasonal flu shot. Moderna said it’s planning early trials of these kinds of combined shots this year. Other combinations of vaccines are already frequently used to immunize younger children against multiple diseases in a single doctor’s visit.
However, administration officials say no decision has yet been reached on how booster shots would be used — or whether they would even be needed.
What about variants?
While booster shots renew the body’s immunity to the virus by mimicking parts of the original strain first identified in China, vaccine makers are also trying to tweak their doses to address newer variants of SARS-CoV-2, some of which are spreading more quickly and may cause more severe illness.
This isn’t unusual; seasonal flu vaccines are regularly changed to address mutations spotted in the virus around the world.
Dr. John Mascola, head of the Vaccine Research Center at the National Institute of Allergy and Infectious Diseases, says understanding SARS-CoV-2’s mutations is “a major focus” for federal scientists.
The NIH has devoted funding and researchers from across its campus to answering key questions about variations in the virus. Some scientists are focused on testing the impact mutations could have on vaccine efficacy. Others are working to better understand and map its “epitopes,” spots where antibodies can target SARS-CoV-2’s signature spike protein.
“That’s sort of a basic scientific body of knowledge that, in the long run, can guide antibody therapies but also guide vaccine design. Basically saying, ‘Can I understand how the virus is going to escape and can I account for that,'” Mascola explained.
Moderna and Pfizer are both pursuing possible versions of their doses adjusted for the B.1.351 variant first spotted in South Africa, though research so far suggests their current vaccines may remain mostly effective against the mutant. The AstraZeneca-Oxford vaccine, which isn’t authorized for use in the U.S., has been found to provide only “minimal” protection against the South African variant.
“The reason they are choosing that strain is it’s one of the ones we know about now, with the variants of concern that are out there, that’s the most antigenically different,” said Mascola.
Mascola also raised the possibility that developing a booster with the South Africa variant could provide more protection.
“For example, if we boost with the B.1.351 strain and we see that the serum antibodies are broader, not only do they neutralize the original strain but also B.1.351 and other variants, then that may be a preferred approach,” added Mascola.
Skipping the needle
There’s also a substantial effort underway to come up with vaccines that don’t rely on needles and syringes to be administered, after record demand strained the complex global supply chain amid the pandemic. Some projects could make it easier to store and transport the vaccine, without the expensive freezers and dry ice currently required for the Moderna and Pfizer vaccines.
For example, future doses could be inhaled through the nose instead of shot into arms. The NIH recently touted promising results from a single-dose intranasal vaccine tested on monkeys, similar to AstraZeneca’s.
The Biomedical Advanced Research and Development Authority (BARDA) last year also announced millions of dollars in contracts to develop a handful of other alternatives delivered by wearable patches or pills, deploying the agency’s experts to shepherd developers through early trials and regulatory approvals.
Vaxess Technologies claims its self-applied patch is shelf stable and painless, delivering its vaccine through microscopic “projections” that dissolve into the skin.
“We’re working with the companies, with the different technologies, to potentially partner them with the six vaccine candidates that are currently being supported by the U.S. government,” said BARDA Director Gary Disbrow.
BARDA hopes the firms can show in smaller trials that they trigger the same kind of immune response as the currently authorized vaccine doses, which could speed their availability to the general public.
“The technologies have been shown for other viral pathogens, but we are trying to support them for the clinical trials. And again, the timing is really dependent upon whether we can identify those correlates for protection,” added Disbrow.
A “pan-coronavirus” vaccine
Scientists at the Walter Reed Army Institute of Research recently announced early trials of a vaccine relying on a “spike ferritin nanoparticle” that has shown some promising results against variants of SARS-CoV-2 as well as the earlier, related virus known as SARS-CoV-1.
“Over the last four years, we’ve been working on trying to move away from one virus, one vaccine. And try to really have vaccines for the future,” says M. Gordon Joyce, a top scientist at WRAIR’s emerging infectious diseases branch.
Unlike the other currently authorized vaccines, WRAIR’s experimental doses are designed to deliver engineered triplets of the spike proteins they hope will train immune systems to produce a greater quantity and diversity of antibodies. Similar to other classic “protein vaccines,” developers say these doses could prove to be sturdier than vaccines that require carefully controlled climates to keep stable.
The researchers say they are in talks with commercial partners for possible next steps for their shots. The current batch of doses being tested could be developed into a “variant-proof” vaccine, booster shots, or serve just as a “proof of principle” for future vaccines aimed at broader groups of coronaviruses.
“We didn’t think that we would already be here with a pan-SARS-like virus vaccine, but it appears we may be there,” says Kayvon Modjarrad, director of WRAIR’s emerging infectious diseases branch.