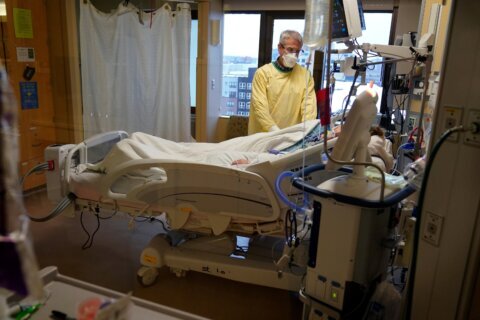
If your health insurance carrier operates in Maryland, and you were given monoclonal antibody treatments for COVID-19, you can’t be billed for the administration of the therapy.
Maryland Insurance Commissioner Kathleen Birrane explained why she invoked emergency powers to require Maryland health insurers to cover Bamlanivimab, Casirivimab and Imdevimab, all used to treat the coronavirus.
Birrane told WTOP that the state wanted to make sure that “providers aren’t reluctant to provide this therapy because they’re concerned about the cost of administration.”
The federal government has supplied states with doses of the various therapies at no cost. But there are costs associated with the administration of the antibodies.
“This is not a shot in the arm,” explained Birrane, “This an infusion therapy that takes place in an infusion center.” She added, “This therapy is still investigational. It’s being allowed under an exception by the FDA.”
But Birrane wanted to make sure that the costs of administering the therapy wouldn’t result in people not being able to get the treatment.
So health insurance carriers in Maryland have been told, “You have to cover this, you can’t claim that it’s experimental, and when you cover it, there can be no cost sharing,” Birrane said. So 100% of the cost of administration has to be covered by the insurance company.
Birrane says many insurance carriers have been voluntarily covering the costs, but her office acted to make certain that it doesn’t become an issue for patients who have insurance that’s issued in Maryland.
You can find more information on monoclonal antibodies from the Maryland State Department of Health, Birrane said.
“If people have any questions, that’s exactly the kind of thing we are here for.”