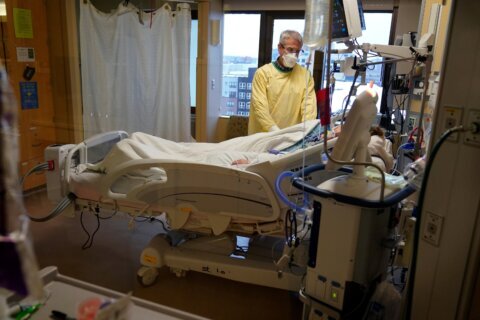
Since contracting COVID-19 back in January 2021, Ken Todd has never made a full recovery, making him one of the millions who suffer from “long COVID.”
“In everyday conversation people say, ‘Hey, how are you?’ Or in emails, ‘Hi, hope all is well.’ And those conversations and those questions are really hard for me to answer.”
CBS News’ chief medical correspondent Dr. Jonathan LaPook asked, “What do you answer?”
“I say, ‘Well, I’m doin’ all right.'”
For Todd, “all right” is very much a relative term. The CDC defines long COVID as health problems that persist more than a month after a COVID infection. For this 53-year-old media executive, long COVID is very much a fact of life. “It’s very discouraging,” he said. “I was doing everything I was told to do. The doctors told me, however, that I would not see improvement over the course of weeks, it would be more like over the course of months. You know, it’s very isolating. You feel like you’re disconnected to the world. The world is moving on without you. And you kind of feel invisible.”
“That’s a terrible feeling,” said LaPook.
“It is.”
Todd works for CBS’ parent company, Paramount Global, but we met him through Survivor Corps, a long COVID patient support organization.
Todd used to be a cross-fit fanatic, but a month after contracting COVID, he found even a stroll in the park would exhaust him. But he did not experience shortness of breath or chest pains: “Nope. Just a weird feeling. I went home and I slept for probably a couple of hours, and then felt better. But that was really the beginning of realizing that something different is going on here.”
What’s been going on are the unresolved (and to outside appearances largely invisible) consequences of COVID-19. For Todd, that means fatigue, dizziness, an inability to regulate his body temperature, and difficulty concentrating. Those are among the most typical symptoms – though chest pain, palpitations, and shortness of breath are also commonly reported.
At NYU Langone Health (where LaPook is a professor of medicine), Dr. Leora Horwitz has gone from treating patients during the worst of the pandemic to searching for a way to diagnose and treat long COVID.
But, she says, you cannot diagnose long COVID based off a blood test, an X-ray, a CAT scan, an MRI, a brain scan or a physical exam.
“You can imagine how that would be disconcerting to somebody who has some symptoms?” asked LaPook.
“Yes, indeed,” said Horwitz. “The scientific community needs to quickly understand what’s going on, needs to quickly make some criteria – some diagnostic rules.”
Horwitz is helping to guide a $1 billion study run by the National Institutes of Health called Recover, and its goal is to learn why so many people who contract COVID-19 are reporting long-term symptoms.
“I’ve been in research for 25 years. I have never seen a study of this scale and this scope start in such a short amount of time,” Horwitz said.
“Why do you think this is taking off quicker than usual?”
“Because COVID is an emergency.”
Consider this: the Centers for Disease Control reports more than half of all Americans have been infected with COVID-19, and as many as one-in-five infected adults have experienced a symptom suggestive of long COVID. That’s tens of millions of people.
Here are a few things we do know:
- The more severe and prolonged the initial experience with COVID, the greater the risk of long COVID;
- Being vaccinated lowers the risk of severe illness and the risk of long-term effects.
But more than two years into the pandemic, researchers still have very few solid answers.
The NIH’S Dr. Walter Koroshetz is at the helm of the Recover study. “The big surprise in COVID has been people who are never even that sick in the acute phase that are still having persistent problems.”
For Koroshetz, who specializes in diseases of the nervous system, the mysteries of long COVID present a familiar dilemma: “I’m a neurologist. A lot of the illnesses that we treat, they don’t have a treatment. Our job is to kind of help people get, you know, as best they can get through their illness. That skill is necessary now more than ever.”
Researchers are honing in on some possible causes of long COVID, including:
- Long-term damage from the initial illness (such as inflammation in the heart, lungs, and blood vessels);
- Disruption of the microbiome (the trillions of bacteria in our gut that have wide-ranging effects on our health);
- The immune system mistakenly attacking healthy tissue after the virus is gone; and
- An immune reaction to remnants of the COVID virus that can remain in the body months after an initial infection.
These last two theories point to similarities with other infections, such as Lyme and Epstein-Barr, which NYU-Langone’s Horwitz says can be difficult to diagnose, just like long COVID. She said, “I want to be very clear about this: The symptoms and the disease are absolutely real. We are failing right now as physicians in figuring out how to identify that and how to characterize it.”
LaPook asked, “I can imagine that the millions of people out there who, for years, have been told, ‘Oh, your chronic fatigue syndrome, your fibromyalgia, your chronic Lyme, it’s in your head’ – they’ve been told that incorrectly, they’re watching this and thinking, See?”
“That’s right!” Horwitz replied.
When Dr. LaPook interviewed Camille Hlavka, of Queens, New York in April 2021, she was struggling to breathe four months after contracting COVID, though doctors said her lungs appeared to function normally.
“A year ago, your son, Reid, was two then?” LaPook said. “You couldn’t really read to him?”
“Yeah. I feel some people might say, ‘Oh, that’s so small and it doesn’t matter.’ But that’s heartbreaking, you know?” Hlavka said. “You never want to deprive your child of something that they love.”
Since then, the 39-year-old Hlavka has made remarkable progress. Medication and breathing exercises helped her run a 10k race last year, and she’s in training for this fall’s New York City Marathon. Some patients feel better with physical therapy and with medications that relieve symptoms, but there are no drugs yet that specifically treat long COVID.
LaPook asked, “From a scale of one to 100, if 100% is where you were before you got COVID, where do you think you are now?”
“I’d say about 80-85%,” said Hlavka. “To everybody, I look, I feel, I seem normal. But the internal struggle that I feel of, you know, a little bit of loss or fear of getting older and the potential that this could get worse again, and that’s, you know, worrying about a ‘what if.’ I think all those little things contribute to the 15%.”
“What would you like to say to people out there who are struggling with long COVID right now?”
“I would like to say that life carries forward,” she replied. “And, you know, as hard as it is that it happened to you, we are alive. Hope is my message – hope.”
That sense of optimism is what propels Ken Todd as well. Though he reports feeling only about 50 percent back to his pre-COVID health, he has improved his stamina by following a physical therapy program developed by New York’s Mount Sinai Hospital.
And he recently volunteered for the NIH’s Recover study. Giving help to others, it seems, gives Todd hope for the future even when the present remains a struggle.
“Whatever I can do to help the medical community figure this out, I want to be able to do that,” he said. “It gives me purpose to talk about my experience. Everybody wants the pandemic to be over. The pandemic is far from over for me.”