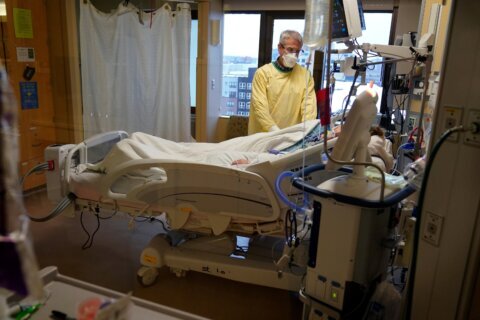
Early research suggests immunity to the coronavirus that causes Covid-19 can last for at least six months — and possibly much longer, perhaps even years, when all components of the body’s immune memory are taken into consideration.
The pre-print paper, posted on Monday to the online server biorxiv.org, adds to the body of research on immunity to the novel coronavirus. Several studies have focused on antibodies, or protein components of the immune system, and some suggested immunity could wane over just a few months.
Yet the new study, which has not been peer-reviewed or published in a scientific journal, involves analyzing multiple compartments of immune memory over time: antibodies, B cells and T cells, among other features of immune memory.
The study included 185 adults, ages 19 to 81, in the United States who had recovered from Covid-19. Most of the adults had mild disease.
The researchers — from the La Jolla Institute for Immunology, University of California, San Diego, and Icahn School of Medicine at Mount Sinai — analyzed blood samples collected at various points following the onset of symptoms, with some collected more than six months later.
In the blood samples, the researchers examined components of immune memory. They found that antibodies “were durable” with only “modest declines” emerging at six to eight months, but noted that there was about a 200-fold range in the level of antibody responses among the adults.
The researchers also found that memory B cells were detected in almost all Covid-19 cases, and there appeared to be an increase in memory B cells over time. “B cell memory to some other infections has been observed to be long-lived, including 60+ years after smallpox vaccination, or 90+ years after infection with influenza,” the researchers wrote in their study.
The researchers identified two types of T cells and their data suggest that “T cell memory might reach a more stable plateau, or slower decay phase, later than the first 6 months post-infection,” they wrote.
The study comes with limitations, including that more research is needed to determine whether similar findings would emerge among a larger group of people across more time points.
“Overall, this is an important study confirming the existence of immune memory to SARS-CoV-2 but with a degree of variation from person to person,” Lawrence Young, professor of molecular oncology at the University of Warwick, said in a written statement distributed by the UK-based Science Media Centre on Wednesday. SARS-CoV-2 is the name of the novel coronavirus.
“This variation might be due to some individuals having had very low-level asymptomatic infection. It might be expected that those previously infected individuals with a low immune memory response would be susceptible to re-infection with SARS-CoV-2,” said Young, who was not involved in the new study.
“But the significant take home message is that the immune response to the virus is more long-lived than previously thought, and this lets us continue to hold hope that an effective vaccine will be able to induce sustained protective immunity.”
Just how much more long-lived than previously thought remains to be seen.
When it comes to other viruses, one bout of measles usually leaves someone immune for life — an effect known as sterilizing immunity. The same was true for smallpox, before that virus was eradicated in the 1970s by a global vaccination campaign. And proper vaccination against measles and smallpox completely protects against infection.
But respiratory viruses such as influenza are trickier. People can catch flu over and over again and flu vaccines generally provide only partial protection against infection and severe disease. Part of that’s due to flu’s tendency to mutate.
Coronaviruses seem to fall in between. There are seven known coronaviruses that can infect people and SARS-CoV-2 is just one of them. Many human coronaviruses can cause the common cold, but because they are not usually deadly, they are not as well studied.