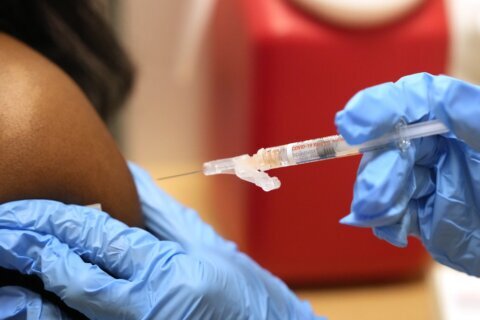
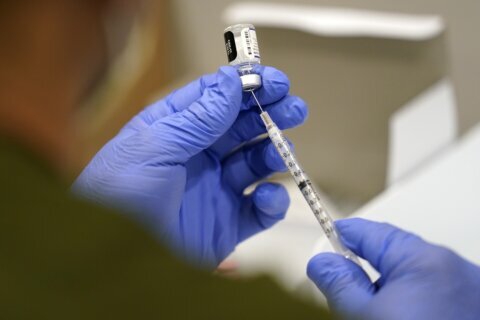
▶ Watch Video: Fauci says new COVID-19 variants “are of concern”
The Centers for Disease Control and Prevention is now tracking the rise of another COVID-19 variant known as BN.1, according to figures published by the agency this month, marking the latest new Omicron descendant now spreading around the country this fall.
Some 4.3% of new COVID-19 cases nationwide are now linked to the BN.1 variant, according to “Nowcast” estimates released on Friday by the CDC.
Prevalence of the new strain is largest in the West, in the region that spans Arizona, California, Hawaii, and Nevada. 6.2% of new cases in that area, HHS Region 9, are from BN.1.
News of the new variant comes as the nationwide pace of new COVID-19 hospitalizations, which had been falling since September, has begun to inch up again over the past few weeks.
A CDC official said Saturday at a webinar hosted by the Infectious Disease Society of America that BN.1 is estimated to be doubling in proportion roughly every two weeks across the country, though they cautioned that early estimates remain muddy.
“The uncertainty in that doubling time is a little higher because the absolute number of sequences is low, because the proportions are low, so has much larger confidence intervals,” the CDC’s Natalie Thornburg said.
Scientists first designated the BN.1 strain back in September, from descendants spotted in Europe and Asia of the BA.2.75 variant.
Some BN.1 strains carry mutations that could result in “high immune escape,” according to predictions from a tool designed by the Fred Hutchinson Cancer Center’s Bloom Lab.
All BN.1 strains carry a change dubbed the R346T substitution, which Thornburg said “we see in a lot of the circulating viruses right now.” That mutation to the spike protein of SARS-CoV-2 could thwart a key medication used to protect people with weakened immune systems.
BQ.1, BQ.1.1, and XBB
BN.1 joins a crowded field of emerging Omicron variant descendants that have swelled in recent months, overtaking the BA.5 variant that had dominated cases over the summer.
The BQ.1 and BQ.1.1 variants remain the most prevalent of the recent new strains. Close to half of infections nationwide are from one of the two, in the CDC’s estimates.
“Our best estimate is that it’s doubling about every 10 days. So if you do the math, BQ.1.1 is likely to become dominant in the next months,” Dr. Ashish Jha, the White House’s top COVID-19 official, told CBS News last month in an interview.
Another variant that had been watched closely abroad – XBB – has yet to reach large enough levels in the U.S. to merit being listed as a standalone strain. Thornburg said Saturday that the CDC still estimated XBB at less than 1% nationwide.
However, the CDC’s variant surveillance in international airports has spotted growing numbers of XBB in arriving travelers so far: 13% of samples through late October were from XBB, 30.4% were from BQ.1 or BQ.1.1, and none were from BN.1.
Findings announced by Moderna on Monday from its updated COVID-19 booster shot suggests the new vaccines may still offer at least some protection against BQ.1.1.
At the Saturday webinar, Thornburg said the CDC is also working on releasing “very soon” new real-world data on the effectiveness of the bivalent shots against the current strains so far.
But the rise of the new strains threatens to bench other key tools used to treat and prevent COVID, especially for more vulnerable Americans.
The National Institutes of Health’s COVID-19 Treatment Guidelines panel warned last week that new variants could evade some COVID-19 treatments like Eli Lilly’s monoclonal antibody, bebtelovimab, urging clinicians to stop using the drug in regions where these strains were dominant.
That now includes the New York and New Jersey region, where the CDC estimates that BQ.1 and BQ.1.1 now make up a majority of infections.
The rise of these and other evasive Omicron variants also threatens the protection offered by AstraZeneca’s Evusheld, the panel warned, which had been a key tool to protecting immunocompromised Americans.
Jha said it could take up to six months for companies to develop new versions of their drugs to counter the latest variants. He blamed Congress for not passing funding which could have subsidized proactive development of new formulations.
“I can’t say I’ll pay for it through the U.S. government, because we don’t have the money and they know it,” said Jha.