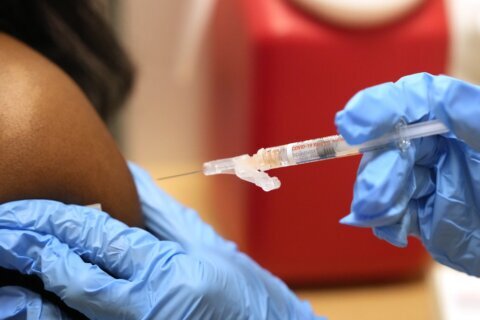
▶ Watch Video: Doctor on COVID-19 surges and need for data on natural immunity
Republican lawmakers in several states have launched efforts to add exemptions to vaccine requirements for people with so-called “natural immunity” from a previous COVID-19 infection. They’re doing so despite evidence that vaccination can cut the risk of COVID-19 even for survivors of the disease, and the fact that there’s no easy way to measure the protection offered by a prior infection.
“Unlike what you see going on with some of the federal proposed mandates, other states, is we’re actually doing a science-based approach,” Florida Governor Ron DeSantis said last week.
The Florida Republican signed a bill he touted as the strongest “anti-mandate action taken by any state.” It includes “medical evidence that the employee has immunity to COVID-19” among a list of exemptions employers must allow in their COVID vaccination policies.
“We recognize people that have natural immunity. You have natural immunity. Whatever a private employer wants to do, you’re automatically exempt because of natural immunity,” said DeSantis.
Florida joins other GOP-led states like West Virginia and Arkansas in requiring employers to carve out a release for workers with “natural immunity.”
In Alabama, the state’s attorney general is urging the legislature to take up the issue. Republicans in Idaho, New Hampshire, Ohio, South Carolina, Texas, and Wyoming are also pursuing bills seeking to protect unvaccinated employees who can show they survived a prior infection, among other excluded groups.
Though the Republican governor of Arkansas, Asa Hutchinson, said last month he would not veto a bill that included the exemption, allowing it to pass into law, he also refused to sign the measure, calling it “unnecessary” and “harmful to our goal of encouraging vaccines.”
“I am opposed to the current mandate by the Biden Administration, but the solution is not to place additional mandates on employers at the state government level. The solution is not to put employers in a squeeze play between state and federal law,” Hutchinson said in a statement.
Proving immunity
There is “clear evidence” that surviving a bout of the disease can result in antibodies that are “approximately equivalent” to two doses of Pfizer or Moderna, the CDC concluded in a science brief last month.
However, not everyone who survived the disease will be able to avoid reinfection or spreading it to others. Measuring whether someone has enough antibodies to offer protection comparable to vaccination remains out of reach for most Americans.
The CDC’s review found a “wide range” of antibody levels in people who recovered from the virus, compared to a typically higher and more consistent antibody response in those who received the vaccine.
So far, the Food and Drug Administration has only authorized serology tests to show whether it was likely someone has been exposed to SARS-CoV-2 in the past — not to verify if they have protection against a reinfection.
The kinds of resource-intensive “neutralizing antibody” tests on blood samples that can be used to attempt to answer that question are currently reserved largely for scientists in clinical trials. Researchers draw blood from participants, then analyze data collected from challenging the body’s antibodies in test tubes against different SARS-CoV-2 variants or dummies carefully designed to mimic the virus.
“It will almost certainly never be done in a commercial lab. It requires lots of setup that’s beyond any commercial scale,” says Dr. Myron Cohen, director of the University of North Carolina’s Institute for Global Health and Infectious Diseases.
Instead, Cohen predicts laboratories in the coming months could soon find better benchmarks that can correlate results from commercial-grade tests with their more demanding counterparts in research labs. That breakthrough will be especially important for doctors treating the millions of immunocompromised Americans who may not have mounted an immune response to their initial shots.
A spokesperson for Roche, which manufactures two popular antibody tests that were authorized by the FDA last year, said the company has launched studies “in recent months” aiming to define a “correlate of protection” measuring whether “an individual is protected from Covid-19 in the future.”
“All this needs to be worked out, so we can decide to whom to give monoclonal antibodies every few months and to whom we can trust the vaccine,” said Cohen.
Further complicating interpretations of current antibody tests is the rapid evolution of the virus itself, which might be able to evade the body’s defenses if the person had previously survived a different variant of the virus.
One recent study published by the CDC, analyzing records of people hospitalized for COVID-19 symptoms through the Delta variant’s dominance in September, found the odds of testing positive was more than 5 times higher among “unvaccinated adults with previous SARS-CoV-2 infection” compared to those who were fully vaccinated with Pfizer or Moderna.
“At least right now, if you had COVID-19, particularly if you had it months and months ago, it’s probably a good idea to get vaccinated,” Dr. Peter Marks, the Food and Drug Administration’s top vaccines official, told a recent webinar hosted by the American Medical Association.
“This is not like getting measles back in March. If you had measles back in March, you’re probably going to be immune now, but that’s not the true thing for COVID-19,” said Marks.