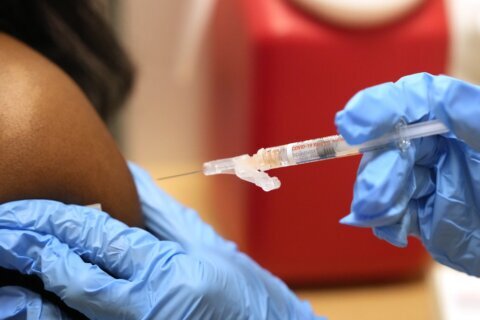
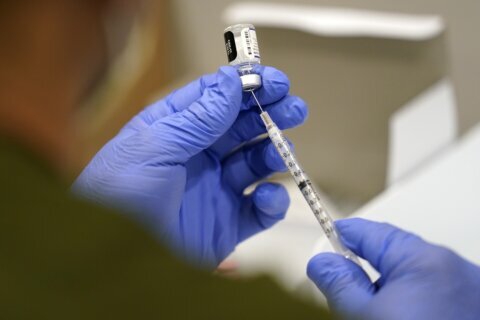
▶ Watch Video: Doctor discusses testing for COVID-19 variants and Johnson & Johnson’s vaccine
U.S. drug maker Emergent BioSolutions began speeding up its acquisition of drug supplies beginning early last year, as the coronavirus outbreak was erupting in China. In addition to producing drugs like the opioid overdose-reversing Narcan nasal spray, the firm develops vaccines and antibody therapeutics and had scored lucrative contracts for key biodefense medicines over the decades.
During the Obama administration, the Centers for Disease Control and Prevention awarded the Maryland-based company with a contract worth up to nearly $1 billion in anthrax vaccine doses in 2016.
In late January last year, the company’s executives presented a white paper for federal health officials, that showed the Trump administration how it could enlist the pandemic vaccine factory funded by President Obama nearly a decade ago.
In the wake of the 2009 H1N1 “swine flu” pandemic, the Obama administration poured millions into building and staffing a handful of Centers for Innovation in Advanced Development and Manufacturing (CIADMs) around the country.
Emergent was selected for one such CIADM award in 2012, and was soon tasked with building a site in Maryland designed to swiftly ramp up vaccine production in the case of another, potentially deadlier pandemic.
“H1N1 demonstrated that even some of the world’s largest vaccine companies didn’t have the capacity for population-scale manufacturing of vaccines for pandemics,” Gary Disbrow, director of the Biomedical Advanced Research and Development Authority (BARDA), tells CBS News.
Federal officials say the country’s vaccine manufacturing capacity has reached its limits in responding to the COVID-19 pandemic, as companies have sought to expand production for the some 800 million vaccine doses ordered by the Trump administration last year.
Pfizer has relied on expanding several of its manufacturing sites in the U.S. and abroad to produce doses of its COVID-19 vaccine. Though far smaller than Pfizer, Moderna struck a deal last year with Swiss multinational Lonza last year to make the key ingredient in its vaccine.
And now as Americans clamor for COVID-19 shots that can’t seem to be produced quickly enough, BARDA-approved Emergent will face its first test.
While it awaits a hoped-for emergency use authorization from the Food and Drug Administration (FDA) by the end of the month, Johnson & Johnson says that the key first step of vaccine production will take place at only three sites: its own facility in the Netherlands, a manufacturing subcontractor in India, and at Emergent’s facility in Baltimore.
How Emergent makes the Johnson & Johnson COVID-19 vaccine
Producing Johnson & Johnson’s COVID-19 shot begins in living tissue cultures grown by Emergent, a tricky process, whereby cells are replicated after being infected with a carefully engineered adenovirus, a type of common cold virus that carries SARS-CoV-2’s signature spike protein.
The vaccine is then frozen and shipped off to “fill-finish” facilities. There, it is thawed, diluted, and divided into vials ready to be distributed.
Johnson & Johnson claims making a batch of their COVID-19 vaccine, from first step through packaging, generally takes just 60 to 70 days. By comparison, Pfizer said recently it was working to cut the time to produce its vaccine from 110 days to 60.
Besieged by overwhelming demand, public health officials welcomed news earlier this month of a potential infusion of vaccine supply brought by Johnson & Johnson’s single-dose immunization.
Its doses have another advantage over Pfizer’s and Moderna’s — Johnson & Johnson’s vaccine can be stored at standard refrigerator temperatures for three months, solving logistical challenges that had forced some vaccination sites to trash spoiled Pfizer and Moderna doses and complicated immunization efforts in more rural communities. Their vaccines, which rely on mRNA technology, are much more fragile and require sub-zero temperatures for longer-term storage.
Clinical trial results touted last week by Johnson & Johnson claim the vaccine was 72% effective in preventing moderate and severe COVID-19 infection among U.S. trial participants.
In addition to manufacturing doses for Johnson & Johnson, Emergent has also been churning out the key ingredient for millions of doses of AstraZeneca’s COVID-19 vaccine. And Novavax relied on Emergent’s production lines for doses used in early clinical trials of its COVID-19 vaccine candidate.
But Biden administration officials acknowledged last week they remain concerned about delays in Johnson & Johnson’s production, first raised during the final months of the Trump administration, which was initially promised 10 million doses of the vaccine by the end of February.
“You’re correct, as is the case with other vaccines, we have not found that the level of manufacturing allows us as much vaccine as we need coming out of the gate,” Andy Slavitt, a White House senior advisor, said at a press briefing on February 5.
“Every option is on the table to figure out how to accelerate manufacturing in the event that the FDA does approve the Johnson & Johnson vaccine,” added Slavitt.
Emergent admitted facing obstacles in ramping up production, though saying they remained confident they would be able to fulfill Johnson & Johnson’s order.
“We took a two-plus year, you know, typical timeline and compressed into seven months, so of course we’re going to have challenges. But nothing that was or is insurmountable,” said Sean Kirk, executive vice president of manufacturing and technical operations at Emergent Biosolutions. Kirk did not say what was causing production delays, though.
“This is not making corn flakes”
Both administration officials and Emergent say the company has benefited from aggressive contracting maneuvers like the Defense Production Act, which can accelerate production by forcing suppliers to prioritize orders by the vaccine manufacturers.
The effort now dominates the work of many along the supply chain, down through companies like Michigan-based Grand River Aseptic Manufacturing, which will fill and finish Johnson & Johnson’s vaccine vials. The company’s capacity has been entirely reserved by BARDA and the Defense Department through August.
However, some warn the Biden administration may already be close to maximizing what the Defense Production Act can accomplish, as it seeks to squeeze out more doses from a complex, specialized production effort.
“Sometimes, allocating priorities for the fill-and-finish lines for manufacturers, critical right now, has bumped products in those finish lines that were destined to other patients with some very critical diseases. So it’s just not a final solution,” former Biden COVID-19 adviser Luciana Borio told a House hearing last week.
Disbrow said the agency was “closely monitoring the impact” on other critical medicines and working with pharmaceutical developers “to try to eliminate negative impacts.”
Both Emergent and Johnson & Johnson declined to provide specific figures on how many doses have so far been produced. A Government Accountability Office report last month said Janssen, the Johnson & Johnson subsidiary that developed the vaccine, estimated just 2 million doses would be delivered at the time of the FDA’s emergency use authorization.
Six days after receiving its emergency use authorization on December 11, a Pfizer press release said the company had shipped “all 2.9 million doses that were asked to ship” and had an unspecified “millions more” in its warehouse.
And in that same time frame, General Gustav Perna, chief operating officer of the Trump administration’s COVID vaccine effort, said Moderna shipped “a little bit short of 6 million doses out” in its first week.
Kirk says that the effort to scale up Emergent’s vaccine production was “unprecedented.”
“This is not making corn flakes,” he said. “This is an extremely difficult and extremely complicated process, and it has to be such because it is a highly regulated, appropriately so, manufacturing process in need of a high level of control.”
He added that while the manufacturing process can be compressed, “it’s something that cannot be rushed to the extent to which one would be compelled to cut corners.”